Reply To:
Name - Reply Comment
Last Updated : 2024-04-19 05:46:00
 As more patients continue to be diagnosed with COVID-19, strict warnings have been issued for those who are afraid to disclose their travel histories or signs of suspected symptoms. Already two hospital wards are locked down for quarantining while healthcare staff in these wards have been sent for quarantining. In the event of a flare up, Sri Lanka needs to be equipped with adequate critical care facilities to accommodate COVID-19 patients. This is apart from accommodating patients with other complications who require critical care treatment. Apart from that people who require essential medicines are stranded as expected services promised by the government haven’t reached their doorstep as yet. The Daily Mirror therefore sheds light on the prevailing situation, national plan to expand ICU facilities and the immediate need to control NCDs.
As more patients continue to be diagnosed with COVID-19, strict warnings have been issued for those who are afraid to disclose their travel histories or signs of suspected symptoms. Already two hospital wards are locked down for quarantining while healthcare staff in these wards have been sent for quarantining. In the event of a flare up, Sri Lanka needs to be equipped with adequate critical care facilities to accommodate COVID-19 patients. This is apart from accommodating patients with other complications who require critical care treatment. Apart from that people who require essential medicines are stranded as expected services promised by the government haven’t reached their doorstep as yet. The Daily Mirror therefore sheds light on the prevailing situation, national plan to expand ICU facilities and the immediate need to control NCDs.
Prevailing situation, unusual symptoms explained
Medical experts advice people to adhere to warnings issued by health authorities, thereby keeping in mind to maintain distance between others, wash hands and use appropriate protective gear. With that in mind, the Daily Mirror spoke to Dr. Neranjan Dissanayake, Consultant Pulmonologist at Ratnapura Teaching Hospital to find out the prevailing situation, keeping a tab on unusual symptoms and why people shouldn’t be afraid to disclose their travel histories.
Excerpts :
Q Could there be an upsurge in the spread of this virus? If so, how could we (the citizenry as well as officials) prepare to prevent it?
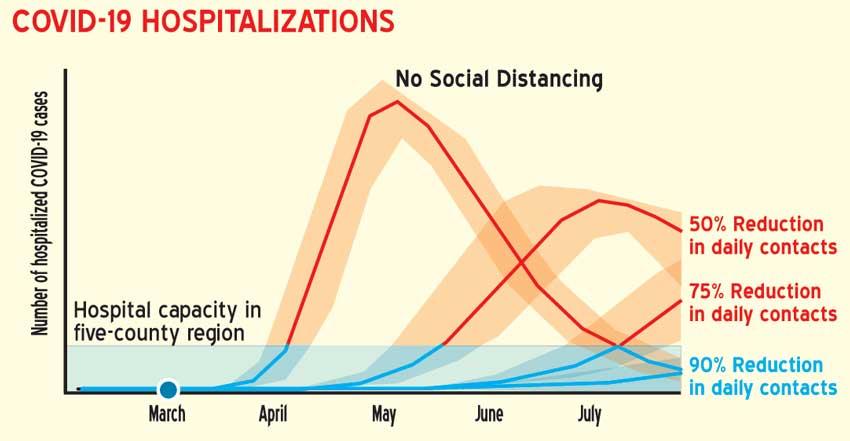
It is very difficult to predict at this moment. It will mainly depend two main factors, among many others. First, the most important is how people will maintain strict social distancing, use proper hand hygiene and use appropriate protective gear to prevent oneself being infected as well as prevent another being infected. It should be practised by at least 90% of the population to make a significant impact (refer graph) to bring the number of patients to a manageable level. But unfortunately, in our country due to many behavioural and socio-economic factors it has been very challenging to implement. The second most important factor is our capability to identify patients early and isolating them before they spread the disease to another. To achieve this, we have to enhance our capacity to identify patients by performing appropriate tests. One very important factor to remember is that in several studies it has shown that up to 30% (One out of three) can be without any symptoms, especially among close contacts. If they are not identified early they have the potential to spread the disease, even without them knowing.
Q There were reports about new s ymptoms such as loss of smell and taste and that patients with this symptom could increase the spread. Could you explain about this?
ymptoms such as loss of smell and taste and that patients with this symptom could increase the spread. Could you explain about this?
Various symptoms have been attributed to COVID 19. The commonest are Fever (99%), tiredness (70%), dry cough (60%), Loss of appetite (40%), muscle pain (35%) and shortness of breath (30%). Some symptoms can be atypical like diarrhoea (10%) and abdominal pain ( 2%). These atypical symptoms might lead to misdiagnosis, resulting in them being admitted without precautions. If this patient is admitted to a surgical ward, for example, he might transmit the disease to other patients and staff who are unaware. A Chinese study has reported exactly that, describing the patient infecting 10 people, 3 who are health care workers.
Loss of smell, or anosmia has been reported in about 40% of people who had viral infections. In Germany 2 out of 3 patients with confirmed COVID 19 had reported loss of smell. In South Korea, 1 out of 3 has had loss of smell as the major presenting symptom. But a peculiar thing about COVID 19 is that especially in US, Italy and France there are reported cases presenting with loss of smell only, with out any other symptoms. This again, if not actively looked for, may result in missing patients with COVID 19, facilitating spread of the disease without knowledge. It is important that we should be vigilant about these unusual presentations to identify these patients early.
Q It seems many people are reluctant to disclose their travel histories due to stigma and discrimination and as a result many areas in the country are on total lockdown. What is your advice to such individuals?
This has been a main issue we face in a daily basis. We all are human beings. None of us want to be discriminated against. Specially, during this pandemic, the measures taken to mitigate the spread might be interpreted by people as discrimination. Hence, they might not reveal these details. This will have severe repercussions. To the patients as well as the staff. To the patient, it will result in a delayed diagnosis or a wrong diagnosis. For the staff as well the other patients, and the health care system as a whole it has major repercussions. It might result in transmitting the diseases to multiple people and will result in whole groups of health staff being sent for quarantine. We will lose these trained professionals, when we need them the most. Hence, I urge from the patients and relatives, please tell us the truth. Help us, to help you.
Q Risks imposed on healthcare staff are seldom spoken about. Apart from PPEs, what other precautionary methods should they follow to minimise themselves from being exposed to the virus?
I must mention and appreciate the incredible work done by our health care workers. From Consultants up to the ladies and gentlemen in the Cleaning services, public health officials and members of the armed forces who are in the frontline of this battle. These trained personnel are an asset to a country and every measure should be taken to protect each and every one of them.
Depending on the risk of exposure and the level of exposure, the protective equipment differs. They are usually trained and advised on the appropriate equipment and how to use them. Hence while taking precautions that were discussed above, where practical, they will be using these equipment and dresses to prevent them from getting infected.
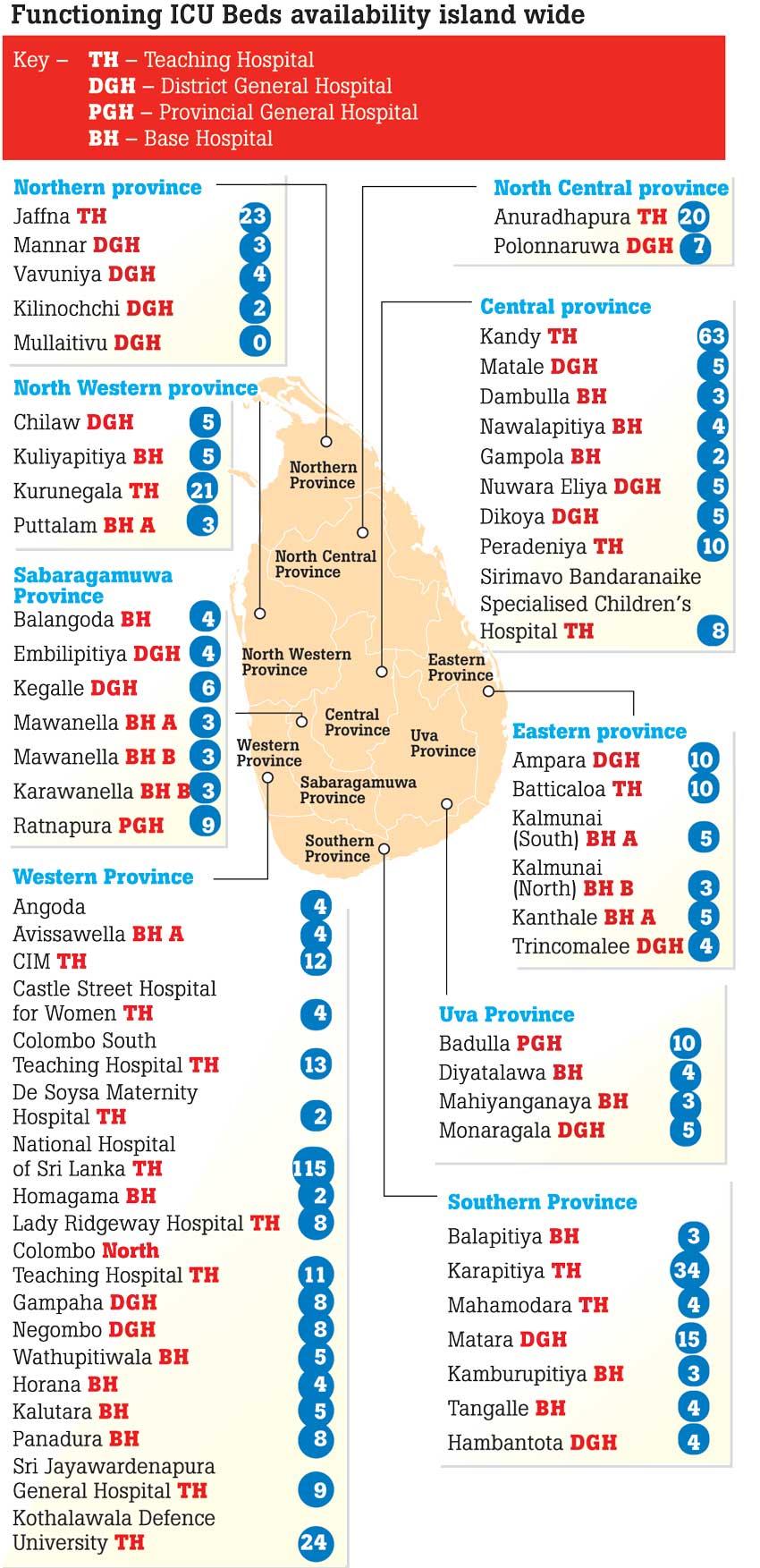
National plan to expand ICU facilities underway
“What we have observed from other countries is that critical care has become the limiting factor,” opined Prof. Vasanthi Pinto, Professor of Anaesthesiology and Critical Care at Peradeniya University. “Therefore the College of Anaesthesiologists and Intensivists have invited interested anaesthesiologists to draw up a national plan. Right now the country is equipped with a little above 600 ventilated ICU beds. According to the plan the IDH Hospital and Mulleriyawa Base Hospital are equipped with ICU beds apart from the newly constructed ICU unit at Kothalawala Defence University which could be expanded if the need arises. Apart from that we are improving ICU facilities at regional level. Therefore the Welikanda Hospital Treatment Unit is also equipped with ICU beds. As part of the plan we also want to mobilise other ICU facilities such as monitors and ventilators because it is not only COVID-19 patients that are there in hospitals. We also need monitors for organ support and patients undergoing renal replacements.” said Prof. Pinto.
“We also need human resources at these units to attend to patients,”she added. “As per the plan in Colombo, Human Resources to function ICU units will be provided by staff from Colombo North, Colombo South Hospitals and National Hospital of Sri Lanka. A new ventilator could cost around Rs. 3 million and therefore we are planning to repair all broken ventilators. Therefore, a multidisciplinary research team from University of Peradeniya which includes experts from the Faculty of Engineering specially from bio-medical, electronic design, electrical, Faculty of Medicine and experts from National Institute of Fundamental Studies have grouped up to find a solution for this national requirement. This team is fully committed to make their best effort to develop a makeshift ventilator within the stipulated time under present circumstance posing many challenges. Once the interface is ready, they can then develop any number of equipment depending on the demand,” the professor said.
She further thanked the Ministry of Health for giving the necessary leadership at this crucial hour.
Medicines to be distributed via Postal Services Department
Apart from groceries and vegetables, medicines are another essential item for many people who are on prescribed drug courses. Despite curfew, desperate customers were queuing up outside pharmacies to find their medicine.
 Therefore, as a direction of the Special Presidential Task Force on Essential Services, medicines are now distributed islandwide with the assistance of the Postal Services Department. “This is done in two ways,” said Postmaster General Ranjith Ariyaratne. “One method is where the respective clinics handover the details of patients registered at government hospitals. They have the patient’s medical histories and know when the patient needs medication next. The prescription and medicines are then handed over to the Postal Department and with the support of regional postal departments, we distribute medicines to their houses. The other method is where we have identified a list of pharmacies that are eligible to distribute medicine. Apart from 40 Osu Sala outlets, 900 other pharmacies could be found on the list. Patients therefore have to use WhatsApp, Viber or IMO and send the prescriptions to the relevant pharmacies. We then deliver the medicines with the bill and both these methods include a service charge of Rs. 75. We are equipped with our personnel to deliver medicines as per the requirement but we are concerned about their safety. Hence we are following adequate safety measures to ensure that our personnel are safe during this period,” said Ariyaratne.
Therefore, as a direction of the Special Presidential Task Force on Essential Services, medicines are now distributed islandwide with the assistance of the Postal Services Department. “This is done in two ways,” said Postmaster General Ranjith Ariyaratne. “One method is where the respective clinics handover the details of patients registered at government hospitals. They have the patient’s medical histories and know when the patient needs medication next. The prescription and medicines are then handed over to the Postal Department and with the support of regional postal departments, we distribute medicines to their houses. The other method is where we have identified a list of pharmacies that are eligible to distribute medicine. Apart from 40 Osu Sala outlets, 900 other pharmacies could be found on the list. Patients therefore have to use WhatsApp, Viber or IMO and send the prescriptions to the relevant pharmacies. We then deliver the medicines with the bill and both these methods include a service charge of Rs. 75. We are equipped with our personnel to deliver medicines as per the requirement but we are concerned about their safety. Hence we are following adequate safety measures to ensure that our personnel are safe during this period,” said Ariyaratne.

Rajya Osu Sala under SPC has taken steps to send medicines to people on request.
Pic by Kithsiri De Mel
Controlling NCDs an immediate need of the hour
 “Apart from experimenting medicine for COVID-19, we need to control non-communicable diseases such as hypertension, diabetes and so forth,” said Dr. Haritha Aluthge, Government Medical Officers’ Association Secretary. “Right now there’s a shortage of insulin. It is a must to control people with NCDs since they could be vulnerable to the virus outbreak. However, even though hierarchical changes have taken place in institutions such as State Pharmaceuticals Corporation (SPC) and State Pharmaceuticals Manufacturing Corporation (SPMC) they still haven’t been able to bring down medicines by pointing out that there’s an emergency shortage. We are not getting ingredients from other countries to manufacture medicines. Although the capacity of patients visiting hospitals has reduced they cannot stop their drug courses,” said Aluthge.
“Apart from experimenting medicine for COVID-19, we need to control non-communicable diseases such as hypertension, diabetes and so forth,” said Dr. Haritha Aluthge, Government Medical Officers’ Association Secretary. “Right now there’s a shortage of insulin. It is a must to control people with NCDs since they could be vulnerable to the virus outbreak. However, even though hierarchical changes have taken place in institutions such as State Pharmaceuticals Corporation (SPC) and State Pharmaceuticals Manufacturing Corporation (SPMC) they still haven’t been able to bring down medicines by pointing out that there’s an emergency shortage. We are not getting ingredients from other countries to manufacture medicines. Although the capacity of patients visiting hospitals has reduced they cannot stop their drug courses,” said Aluthge.
He also identifies an issue with regard to the delivery of medicines. “Most SPC outlets don’t function during weekends. Cancer patients are also facing problems, but that is not as bad as last November when they were short of 20-30 drugs. Since the payments have been done, many of them now have access to cancer drugs except for four or five brands.” said Dr. Aluthge.

Add comment
Comments will be edited (grammar, spelling and slang) and authorized at the discretion of Daily Mirror online. The website also has the right not to publish selected comments.
Reply To:
Name - Reply Comment
On March 26, a couple arriving from Thailand was arrested with 88 live animal
According to villagers from Naula-Moragolla out of 105 families 80 can afford
Is the situation in Sri Lanka so grim that locals harbour hope that they coul
A recent post on social media revealed that three purple-faced langurs near t