Reply To:
Name - Reply Comment
Last Updated : 2024-04-27 00:40:00

Currently dermatologists, not only in Sri Lanka, but also in other South Asian countries have reported a rise in ringworm disease. Despite its name, the disease is actually caused by a type of fungus called a dermatophyte.  While the ringworm disease is a common skin disease, the unusual rise of it and it being non-responsive to the traditional treatment methods resulting in its increased extensiveness has alarmed dermatologists in the region. In this backdrop, Daily Mirror spoke to Consultant Dermatologist at National Institute of Infectious Diseases, Dr. Nayani Madarasingha and Consultant Dermatologist at Lady Ridgeway Hospital, Dr. Sriyani Samaraweera.
While the ringworm disease is a common skin disease, the unusual rise of it and it being non-responsive to the traditional treatment methods resulting in its increased extensiveness has alarmed dermatologists in the region. In this backdrop, Daily Mirror spoke to Consultant Dermatologist at National Institute of Infectious Diseases, Dr. Nayani Madarasingha and Consultant Dermatologist at Lady Ridgeway Hospital, Dr. Sriyani Samaraweera.
Occurrence of Ringworm Disease
 “This is a common skin disease where the fungus affects the keratin containing cells (skin, hair and nails). The fungus affects the superficial skin layer thus the disease is not fatal,” stated Dr. Madarasingha.
“This is a common skin disease where the fungus affects the keratin containing cells (skin, hair and nails). The fungus affects the superficial skin layer thus the disease is not fatal,” stated Dr. Madarasingha.
The symptoms of the disease can differ according to the site of infection, according to Dr. Madarasingha. A red round patch with a usually clear center, margin with red bumps and extensive scaling can be seen when the infection occurs on the skin. This is mostly seen on flexures but can be widespread too. When scalp is infected, red scaly patches and areas of hair loss are seen. When toe webs are infected, a whitish thick plaque-like material is visible between the toes and blisters too could develop after some time. Redness and scaling may also be present in the palms or the soles.
“One of the possible reasons we believe that the disease has risen in the South Asian region is due to the current 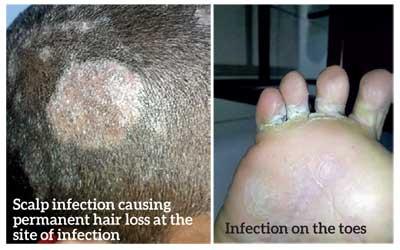 hot and humid weather,” opined Dr. Madarasingha. Other causative factors for this disease are poor personal hygiene, wearing tight fitting clothes and wearing closed toe shoes for a long period of time. She also revealed that immuno-compromised people such as those with diabetes, cancer and those who have recently had an organ transplant have a higher risk of contracting the disease.
hot and humid weather,” opined Dr. Madarasingha. Other causative factors for this disease are poor personal hygiene, wearing tight fitting clothes and wearing closed toe shoes for a long period of time. She also revealed that immuno-compromised people such as those with diabetes, cancer and those who have recently had an organ transplant have a higher risk of contracting the disease.
Dr. Samaraweera noted that children can develop extensive ringworm infections due to affected close contacts. However, animal ringworm infections were most commonly seen in children due to children being exposed to infected pets. “Scalp animal ringworm infections give rise to an inflammatory boggy mass in the scalp. On healing, it may cause permanent hair loss,” she revealed. Dr. Samaraweera added that even adults are susceptible to animal ringworm infections which are commonly transmitted via infected pets.
Both doctors stated that ringworm disease is mostly transmitted via person to person contact. The disease can be transmitted through sharing of clothes, towels and beddings with an infected person. Even coming in contact with the surfaces touched by the infected person can cause the transmission of the disease.
 Reasons for the increasing extensiveness of the disease.
Reasons for the increasing extensiveness of the disease.
Due to the itchy nature of the disease, the infected person may seek quick relief for it. Often, this results in them obtaining certain combination medications which contains anti-fungal drugs and steroids. This could lead to steroid abuse. Dr. Madarasingha stated that these drugs are prescription medication but in Sri Lanka, are available for purchase without a prescription in pharmacies. “These drugs provide quick relief but causes the disease to become extensive which would result in longer treatment duration and can also be difficult to treat,” cautioned Dr. Madarasingha. In the past, the combination medication also included a triple combination of antibiotics, anti-fungal drugs and steroids but currently such triple combination medication has been banned in the country for causing increased extensiveness in fungal skin infections. “The newly registered products have been banned yet the ones registered before the ban are still available in the market. These products cause the infections to worsen,” she said.
She also stated that anti-fungal resistance can be a causative factor for the increasing extensiveness of the disease. This occurs due to people not following the treatment for the prescribed time period as some stop medication when the symptoms of the disease disappear within a few days of treatment. Dr. Madarasingha warned that though the symptoms disappear, it does not mean the patient is fully cured therefore a re-emergence of the disease could occur and it could be more extensive. She also said that anti-fungal resistance can also be caused as a result of exposure to fungicides.
Dr. Samaraweera noted that anti-fungal resistance was a worldwide phenomenon as many fungal infections are becoming resistant to the anti-fungal drugs that were used to treat these infections.
Overcoming the issue
Currently in Sri Lanka, dermatologists and mycologists are working hard on overcoming this problem. This includes scientific research, liaising with health care policy makers and conducting educational activities. Health education programmes are already underway for doctors to notify them of the current status of fungal skin infections in Sri Lanka and lack of therapeutic response. Minimising steroid misuse among public will play an important role in overcoming this problem.
While no new anti-fungal drugs have yet been discovered to overcome the anti-fungal resistance, Dr. Samaraweera revealed that identification of various species of fungi with skin scrapings helped dermatologists to better manage the condition. “However, awareness of the public is very important. When patients come to the clinic we try to educate them on the disease. In case of children, we educate the parents or guardians regarding fungal skin infections,” stated Dr. Samaraweera.
As preventive measures, Dr. Madarasingha advised the public to follow proper personal hygiene and to avoid sharing clothes. “If infected, it is best to seek medical care during the early stages as it is easier to cure the disease in the early stages,” she stated adding that for mild cases of the disease, topical creams are prescribed while in severe cases, oral anti-fungal drugs are prescribed for a specified period. She reiterated that when infected, one should not self-medicate themselves nor should one discontinue treatment before the specified time duration. Steroids or combination creams with steroids as an ingredient should not be used at any point. “The instructions given by the dermatologist, including repeat visits after a specified duration should be followed. If the condition persists, please visit the dermatologist again,” she stated.

Add comment
Comments will be edited (grammar, spelling and slang) and authorized at the discretion of Daily Mirror online. The website also has the right not to publish selected comments.
Reply To:
Name - Reply Comment
US authorities are currently reviewing the manifest of every cargo aboard MV
On March 26, a couple arriving from Thailand was arrested with 88 live animal
According to villagers from Naula-Moragolla out of 105 families 80 can afford
Is the situation in Sri Lanka so grim that locals harbour hope that they coul

9 hours ago
26 Apr 2024