Reply To:
Name - Reply Comment
Last Updated : 2024-04-27 00:40:00
 The Leprosy Hospital in wattala : A safe refuge for the isolated victims of leprosy
The Leprosy Hospital in wattala : A safe refuge for the isolated victims of leprosy Leprosy was considered a curse in the past and as there was no cure, patients were treated as outcasts and kept in Leper Asylums. Many countries around the world have eradicated leprosy. It was believed to have been eradicated in Sri Lanka as well. Yet, reports show that the disease is on the rise. The importance of making the public aware of the disease led us to the Leprosy hospital in Hendala. Chief Medical Officer of the Hendala Leprosy hospital, Dr. Jayalath Chandrasiri and Director  of the Anti-Leprosy Campaign Dr. Priyantha Karunarathna commented on the spread of the disease.
of the Anti-Leprosy Campaign Dr. Priyantha Karunarathna commented on the spread of the disease.
“A lack of attention paid to changes in the skin is the root cause for the infection worsening. Once treated, patients can no longer spread the disease. The government aims to eradicate leprosy from Sri Lanka by 2020,” emphasized Chief Medical Officer of Hendala Leprosy Hospital, Dr. Jayalath Chandrasiri.
“Leprosy is a slow-spreading airborne communicable disease, caused by the bacteria Mycobacterium leprae. It is a pathogenic bacteria that infects the peripheral nerves. It shares similar features with the tuberculosis bacteria,” explained Dr. Priyantha Karunarathna.
There are two leprosy hospitals in Sri Lanka, situated in Hendala and Maanthivu island (close to Batticaloa). The latter has only one inmate. It is said that a Dutch captain who had leprosy travelled to the present hospital premises which was a shrub-land at the time and settled there secretly. He was brought food from the other bank and relatives built a small structure there for him.
The Dutch VOC hospital opened in 1701 and construction of the buildings was completed in 1708. The inauguration symbol still can be seen there. Since its inception, many leprosy patients were admitted here. The hospital itself is considered an archaeological site and is 309-years- old. The leprosy hospital has the oldest washing machine which was made in England and brought to Sri Lanka in 1938. Most buildings in the hospital premises are in ruins and renovation does not take place since it was declared an archaeological site in 2015. Nobody has the permission to renovate the site except the Archaeological Department.
The Hendala Leprosy hospital is home to 29 leprosy patients living in four wards. They cannot transmit the disease, yet their deformities are clearly visible. They have been neglected by their families. Some of them who are skilled in craft-making are helped by the hospital. A 40- member staff is engaged in looking after the patients along with three doctors. In the past, they had 32 acres of land but this has now been reduced to seven and a half acres. The hospital is maintained by the Health Ministry and warmly welcomes helpless patients who have nowhere else to turn.
Stating the statistics of leprosy in the country, he said, “Last year the number of patients recorded was 1,863 and the majority of cases were reported from the Western Province, with the total patients recorded being 917. In 2015, there were nearly 2,000 reported cases. Usually we do not get patients below the age of 3 as it takes some time for the disease to develop. Patients are usually above the  age of 3 and even above the age of 70. The bulk of patients are between the ages of 25 and 45. Last year the number of children (below the age of 15) recorded was 155.”
age of 3 and even above the age of 70. The bulk of patients are between the ages of 25 and 45. Last year the number of children (below the age of 15) recorded was 155.”
“We are worried about three parts of the country which are considered highly endemic areas. The Western Province, the Eastern Province (Kalmunai, Ampara and Puttalam) and the Southern Province. The majority of patients are in Colombo, Kalutara and Gampaha. In these districts we have observed that it is found mostly among underprivileged families, those in slum areas and the fishing community. The highest number of cases are reported from the Moratuwa area.”
Speaking of public awareness on the disease Dr. Karunarathna said, “We want to spread the message to these areas that if they notice anything resembling this disease, they should seek medical help. The message is not being passed properly. In addition to this, there is a stigma attached to this disease so people don’t speak about it and some even hide it from their family members and do not go for treatment.”
The strength of one’s immune system is the main determinant in contracting the disease.“The weaker the immune system, the higher the chance of getting the disease. The strength of our immune system depends on many things such as genetics, nutrition, general health, the environment, housing, ventillation, congestion and economic status. Thus the lifestyle people lead can determine whether or not they will contract the disease.
The transmission of the disease occurs through respiration, when the bacteria enters the victim’s  nose. The bacterium must enter the person’s body for them to contract the disease. Some epidemiological studies have shown that there is a predominance for the disease in males rather than females but anyone can be affected by the bacterium. A leprosy patient can transmit the disease after a few months to those around him through respiration, sneezing and coughing, where the bacterium is released into the environment. Those around the patient can get the disease this way. It does not spread through contact but mainly through airborne transmission.
nose. The bacterium must enter the person’s body for them to contract the disease. Some epidemiological studies have shown that there is a predominance for the disease in males rather than females but anyone can be affected by the bacterium. A leprosy patient can transmit the disease after a few months to those around him through respiration, sneezing and coughing, where the bacterium is released into the environment. Those around the patient can get the disease this way. It does not spread through contact but mainly through airborne transmission.
A person could inhale the bacteria spread by a patient, however 95% of the time healthy people remain unaffected due to a good immune system and other factors such as genetics and nutrition. Only 5% or 10% of people may get the disease. Factors leading to this includes spending a lot of time with the patient or a weak immune system.
The leprosy bacteria is very peculiar. Once it enters the body, it gradually travels to the nervous system and reaches out to the relatively cooler parts of the body, such as the hands, feet and face. Once they have started replicating, patches will start to appear on the skin and are the earliest sign of infiltration.
Then they invade the sensory nerves closer to the skin and the patient complains about the patch and the anaesthetic feeling around the patch. This might spread all over the body.
It’s crucial to know about the early stages in order to get treatment as soon as possible. The most common symptoms are the patches appearing on the face, hands and feet. The colours of the patches are lighter than the other parts of the skin and may vary from copper to gold. If observed carefully, the sensation of the area having the patch will be less compared to other areas. Identification is done by pricking the spot with a needle.
There may be other variations in the early stages. Sometimes it may appear as a thickened nerve. Patients may feel a lump under the skin on their face, hands or feet, due to the nerve involvement. If such signs persist for more than two to three months, this could be a sign of leprosy. If someone has suspicions about the disease he/she should seek the advice of a dermatologist. Neglecting medical treatment in the early stages will lead to complications.
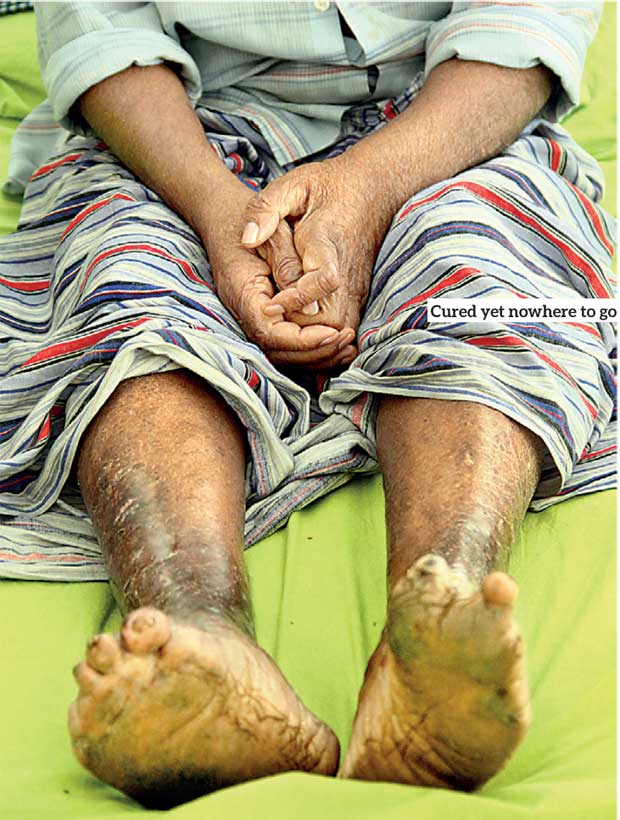
If early stages are ignored, the bacteria can infiltrate the nerves. Sensory nerves and motor nerves connected to muscles can be affected and patients will complain about numbness in their feet and hands. Gradual nerve involvement will lead to deformities. The nerves stop working and the limbs become thick and unmovable.
With the progression of the disease, injuries too will take place. People might get cut or badly burnt because they lose their sense of touch. When the ulcers and injuries do not heal naturally, the body’s reaction is to expel the limbs, fingers or toes, causing these parts to
drop off.
It is important for people to know that treatment is available for leprosy and that it is 100% curable. Usually, if someone has contracted leprosy it is diagnosed by a dermatologist. Leprosy treatments are only available in the government sector, throughout the country in any hospital with a dermatologist. We have ensured that there are no difficulties or barriers to access these services. Private sector dermatologists will direct patients to a government clinic.
Some will have to take this treatment for six months and others for one year. It is a combination of drugs which patients will be directed to use.
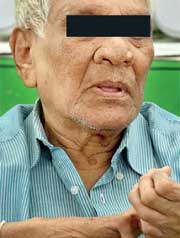 Edward Alwis from Dehiwala
Edward Alwis from DehiwalaWe are told he is the oldest inmate on the premises. He was admitted on April 6, 1943 at age 18. He detected two patches on his face and was later registered at the hospital. “There were 800-900 patients and 22 wards at the time I came. There was a drop in patients after 1956.” Edward says some of them were even sent to jail, as fights would break out for better meals to be introduced. “All my siblings are married but I couldn’t get married because of this disease. People don’t come and visit because they think they will get the disease but we have all been cured, so it won’t spread,” he added
“The waste management in this place should be properly disposed of, assuring health safety. They just dump the bandages and other waste into a garbage dump and burn it. This is not healthy. Some employees don’t have identification cards even though they have worked here for two years. The buildings are very old and have not been preserved. Many are falling to the ground.”
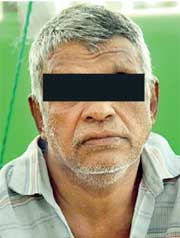 Heen Banda from Kandy
Heen Banda from Kandy“I first detected a numbness in my feet in 2002. I misunderstood it for another disease and got treatment for two years. It was at the government hospital that I realised I had leprosy.” Heen Banda says the wounds caused by leprosy should be well cared for, otherwise the disease would worsen.
Ananda is very skilled in woodwork and was admitted at the age of 18 when he detected scars on his body. He has his own wood workshop, where he takes orders to make wardrobes and other furniture. He also makes special sandals to meet the needs of his fellow patients.
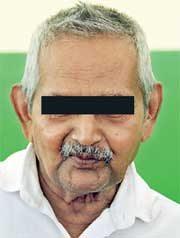 P.B. Doratiyawa from Kegalle
P.B. Doratiyawa from KegalleHe spoke about the lack of facilities there and especially the poor meals. “I’m a vegetarian but they gave me the same thing they gave everyone else.” He was admitted to the hospital in his forties.
“All these buildings are falling apart. Some wards are door-less and dogs come in at night. We have issues with the quality of food we are given here. Even though we are entitled to quality meals, what comes to our plates lacks quality.”
 Kamala Gunathilaka from Bandaragama
Kamala Gunathilaka from Bandaragama“I was admitted in 2001. First I was diagnosed with diabetes and my leg was amputated. I was then taken to the skin clinic where the disease was recognized.” She had been manufacturing envelopes while warded and had to be satisfied with the Rs.500 allowance.
 Peter Hettiarachchi from Kahawatta
Peter Hettiarachchi from KahawattaI came here in 1950, when I was 10-years-old. We were sent back home in 1960 after being told we could not spread the leprosy germ after being given the DDS tablet. We demanded an allowance from them because we had been there for years and that’s how we got the Rs.500 monthly donation.

Add comment
Comments will be edited (grammar, spelling and slang) and authorized at the discretion of Daily Mirror online. The website also has the right not to publish selected comments.
Reply To:
Name - Reply Comment
US authorities are currently reviewing the manifest of every cargo aboard MV
On March 26, a couple arriving from Thailand was arrested with 88 live animal
According to villagers from Naula-Moragolla out of 105 families 80 can afford
Is the situation in Sri Lanka so grim that locals harbour hope that they coul

26 Apr 2024
26 Apr 2024