Reply To:
Name - Reply Comment
Last Updated : 2024-04-27 00:00:00
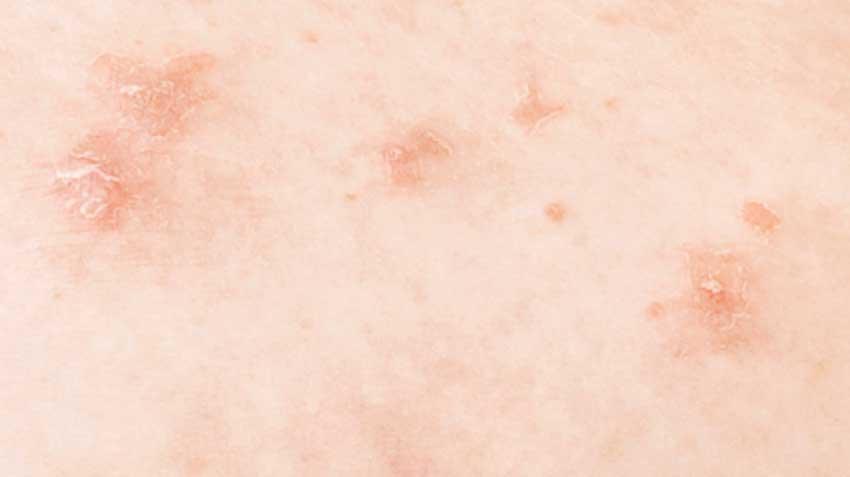
A common symptom of Sarcoidosis is skin rash
 The International Sarcoidosis Awareness Day was celebrated globally on April 13. Understanding the importance of spreading awareness, Daily Mirror spoke to Consultant Pulmonologist Dr.NeranjanDissanayake (MBBS MD (Medicine) MRCP (UK) FCCP (SL) FRCP (London)) to shed some light on the disease.
The International Sarcoidosis Awareness Day was celebrated globally on April 13. Understanding the importance of spreading awareness, Daily Mirror spoke to Consultant Pulmonologist Dr.NeranjanDissanayake (MBBS MD (Medicine) MRCP (UK) FCCP (SL) FRCP (London)) to shed some light on the disease.
Understanding Sarcoidosis
Sarcoidosis is a relatively rare disease of unknown origin affecting many organs with dire consequences if not properly diagnosed and managed. It predominantly affects the lungs, lymph nodes and skin and manifests as “granulomas”, collections of compacted inflammatory cells. In sarcoidosis these granulomas appear without any discernible cause and in exaggerated numbers, infiltrating organs and causing damage and dysfunction of that organ.

“Even after extensive scientific research, we are still at a hypothetical stage on identifying what causes sarcoidosis. It certainly has a proven genetic predisposition, where certain ethnicities such as African Americans and Scandinavians are found to be more affected than others. In Sri Lanka, even though limited research exists, we have seen it more commonly in the Sri Lankan Moor population. Furthermore, certain environmental factors such as infective organisms, inorganic dusts and chemicals such as pesticides have also been implicated,” Dr. Dissanayake said.
“An important facet in the Sri Lankan context, is that Sarcoidosis may mimic Tuberculosis. Both diseases might be similar in its initial presentation with vague symptoms such as fatigue, mild pain in joints and a feverish feeling. Furthermore, when the disease affects organs and systems, sarcoidosis, similar to tuberculosis can affect any organ of our body, predominantly lung and lymph nodes. When a tissue sample is analyzed, both diseases reveal granulomata. So sometimes we are in a diagnostic dilemma, and would rely on expert pathological, microbiological and clinical acumen to arrive at a diagnosis,” he explained.
Signs and Symptoms
There are some distinct collections of presentations labeled as syndromes that have been identified.
“But the commonest are various skin manifestations, such as nodules, rashes, hardened raised fleshy lesions (lupus pernio), enlarged lymph nodes, characteristically at the root of the lung (hilum) and scarring of the lung (fibrosis),” Dr. Dissanayake stated.
Diagnosis and Treatment and Prevention
“As we don’t know the exact cause of the disease, we really can’t prevent Sarcoidosis. The most important thing is identifying it correctly in the earliest stages. Even though it is a relatively rare disease, in the appropriate clinical context, a clinician have to suspect it,” Dr. Dissanayake emphasized.
Radiological imaging (US scans, CT/MRI/PET imaging) , serum calcium levels, urine calcium levels, cell counts/types in bronchoscopy lavages and serum angiotensin converting enzyme levels (ACE) will help in further evaluating a suspected patient. Furthermore, if a biopsy from an affected organ shows well-formed granulomata, it further enhances the probability.
“Not all sarcoidosis patients need treatment. Even after we confirm a diagnosis, sometimes we differ treatment because the treatment may be more harmful than the disease itself for that patient.Hence, we balance the risks and the benefits of treatment and the potential outcome before initiating treatment.”
“Corticosteroids, are a mainstay of treatment. Unfortunately, high doses of steroids can cause significant harmful side effects like diabetes, brittleness of bones, suppression of the immunity and increased risk of heart diseases,etc. There are some other drugs that we use such as anti-metabolites (e.g. Methotrexate, Azathioprine) that can help reduce the steroid dose and the duration.” Dr. Dissanayake explained.
“The duration of treatment also varies, depending on the organ involvement, severity and the response to treatment. We can achieve remission in majority of patients but one in twenty can relapse. Unfortunately,the risk of premature death in these patients is about three times more than the general population and they have a higher tendency to develop certain malignancies as well,” he added.

Add comment
Comments will be edited (grammar, spelling and slang) and authorized at the discretion of Daily Mirror online. The website also has the right not to publish selected comments.
Reply To:
Name - Reply Comment
US authorities are currently reviewing the manifest of every cargo aboard MV
On March 26, a couple arriving from Thailand was arrested with 88 live animal
According to villagers from Naula-Moragolla out of 105 families 80 can afford
Is the situation in Sri Lanka so grim that locals harbour hope that they coul
4 minute ago
4 minute ago

6 hours ago
7 hours ago