
Life with Chronic Kidney Disease (CKD) is a struggle to say the least. CKD is the progressive and irreversible deterioration of the function of the kidneys over a period of time and patients rarely feel sick until their kidney disease is advanced. Due to the increasing number of patients diagnosed with non-communicable diseases like Diabetes and Hypertension which are the main causes of CKD worldwide,CKD has become a major burden for the healthcare system in Sri Lanka.
Dialysis is a treatment option for these patients, a process which takes over the function of the kidneys until the patient finds a suitable kidney donor. In times before dialysis was invented, patients with kidney failure had no choice but accept a slow, painful death with time.
What is dialysis?
Dialysis is the process by which a patient’s blood can be cleaned to get rid of the body’s waste products like urea, creatinine etc., extra salt & water.
There are two main types of dialysis :
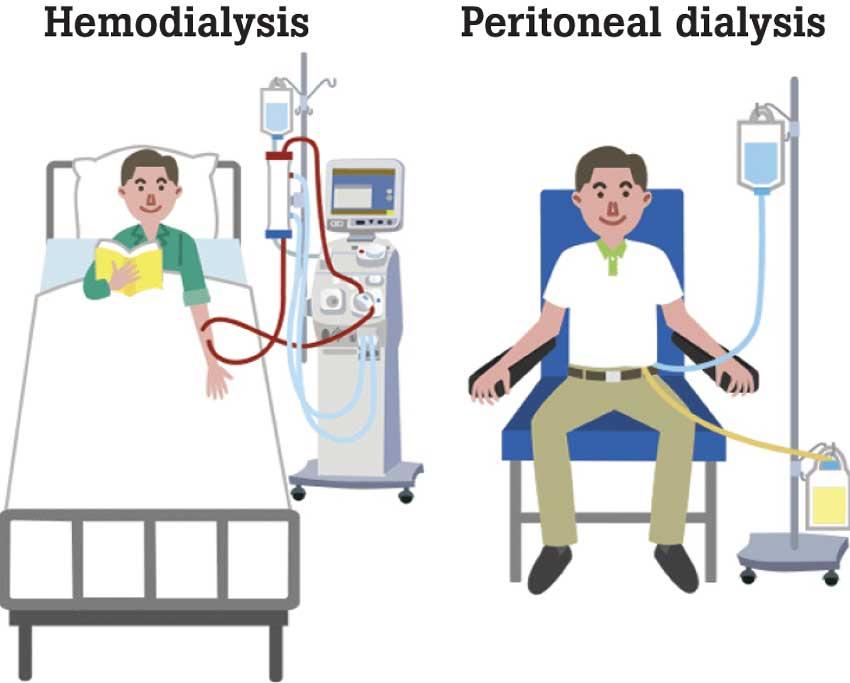
- Haemodialysis
- Peritoneal Dialysis
In haemodialysis (HD), the patient is connected to a dialysis machine via plastic tubes & blood is pumped out of the body via blood vessels to go through a filter in the machine to purify the blood & then returned to the body. This filter acts as an artificial kidney outside the body.
Peritoneal Dialysis – How it works :
In peritoneal dialysis (PD), the inside lining of the patient’s belly, known as the peritoneal membrane, acts as a natural filter. A soft plastic tube called a catheter is inserted into the belly. This catheter is used to put a sterile cleansing fluid called the dialysate into the patient’s belly.
This dialysis solution contains water with a sugar called dextrose/ icodextrin and while it is inside the belly, it absorbs body wastes and extra fluid from the body through the peritoneal membrane. The patient keeps the solution inside the belly for a few hours. While the solution is fresh, it absorbs wastes quickly and as time passes the filtering slows down. Due to this reason, this solution has to be drained out of the belly into an empty bag & the patient has to repeat the process by refilling his/her belly with fresh solution four to six times every day. The process of changing the solution is called an exchange.
What are the types of PD?
There are two types of PD :
- Continuous Ambulatory Peritoneal Dialysis (CAPD)
- Automated Peritoneal Dialysis (APD)
In CAPD, the process is continuous, machine-free and done by the patient himself or a carer by hand. Several exchanges are done during day time while the patient is awake. Each exchange takes about 30-40 minutes & after that the patient can go and engage in normal day to day activities while the solution is inside the belly.
APD differs from CAPD as APD uses a machine called a cycler to deliver & then drain the dialysis solution to & from the patient which is usually done at night while the patient is asleep.
PD vs HD
There are several benefits of being on PD when compared to HD.
Advantages of CAPD
- Patient is independent and mobile.
- Residual renal function is preserved for a longer time.
- Less restrictions on diet & fluid intake.
- No need to access blood vessels.
- Reduced risk of developing low blood pressure & abnormal heart rhythms during dialysis.
- Reduced stress on the heart & blood vessels.
- No need of anticoagulants like Heparin.
- Reduced exposure to viruses like Hepatitis B, C transmitted by blood.
- Reduced risk of bacteria entering into blood to cause infection.
- Reduced need for Erythropoietin & blood transfusion.
However, PD may not be appropriate for some people. PD is not suitable for patients having –
- Multiple scars in the belly
- Adhesions inside the belly causing organs/ tissues to stick together
- Large herniae
- Severe obesity
- Severe COPD
- Enterostomy (intestine diverted to an artificial opening in the abdominal wall)
- Urostomy (urinary diversion by surgically created opening in abdominal wall to pass urine)
How to prepare for PD :
Before the first treatment, a soft plastic tube called a catheter will be placed in the abdomen of the patient by a surgeon under general or local anaesthesia. A part of this tube will be visible coming out of the abdomen and will have a secure cap on the end to prevent infection. Between exchanges the patient can keep the catheter hidden inside clothing.
All supplies needed for PD will be supplied by the healthcare team and both CAPD and APD can be done in a clean, private place in home/ at work or when travelling.
Dialysis training is provided to the patient from the healthcare team to learn how to do exchanges. It’s better to bring a family member or another carer to training in case the patient has a sick day and needs help with the exchanges.
What are the complications of CAPD?
Complications of CAPD can be infectious or non-infectious.
Infectious complications :
- Exit-site infection
- Tunnel infection
- Peritonitis
Out of these, peritonitis is a significant cause of hospitalisation and PD failure. Peritonitis is the inflammation of the peritoneum usually caused by bacterial infection. Common symptoms include pain in the abdomen, distension, nausea, vomiting, fever and cloudy peritoneal effluent when it is drained during dialysis. Therefore, it is always important to check the drainage bag for colour change and cloudiness.
Peritonitis can be treated with antibiotics given via the peritoneal dialysis fluid.If it continues to recur, PD may have to be stopped.
Exit site infections are commonly caused by the bacteria normally residing on our skin. It can cause redness over the catheter exit site, pain and purulent discharge. This can be treated by topical/oral/IV antibiotics as needed. Careful hand washing and wearing a surgical mask while you connect your catheter to the transfer set helps prevent infection.
Other non-infectious complications are catheter dysfunction/obstruction, catheter malposition, fluid leaks, hernia and metabolic complications eg: increased blood sugar, electrolyte changes.
In summary,
CAPD is a good option in centers with limited resources that are overloaded with patients who need dialysis. There are advantages of using CAPD, when compared to haemodialysis and it can be a very successful form of dialysis with careful patient selection.
The writer is a Temporary Demonstrator at
Psychiatry Department
General Sir John Kotelawala Defence University
 Life with Chronic Kidney Disease (CKD) is a struggle to say the least. CKD is the progressive and irreversible deterioration of the function of the kidneys over a period of time and patients rarely feel sick until their kidney disease is advanced. Due to the increasing number of patients diagnosed with non-communicable diseases like Diabetes and Hypertension which are the main causes of CKD worldwide,CKD has become a major burden for the healthcare system in Sri Lanka.
Life with Chronic Kidney Disease (CKD) is a struggle to say the least. CKD is the progressive and irreversible deterioration of the function of the kidneys over a period of time and patients rarely feel sick until their kidney disease is advanced. Due to the increasing number of patients diagnosed with non-communicable diseases like Diabetes and Hypertension which are the main causes of CKD worldwide,CKD has become a major burden for the healthcare system in Sri Lanka.