Reply To:
Name - Reply Comment
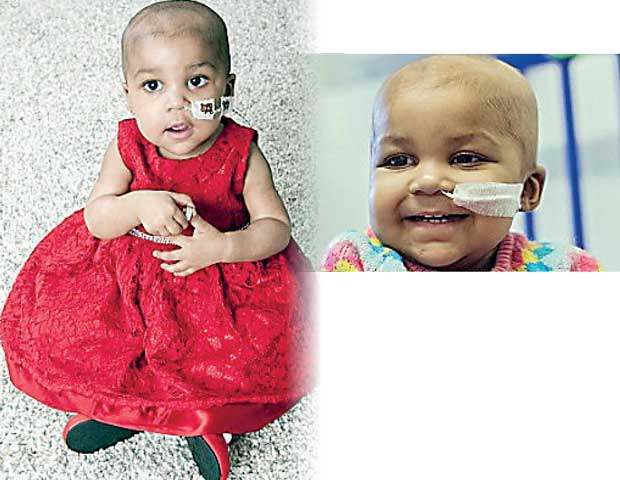
A dying baby whose life was saved by a pioneering ‘designer gene’ technique has remained cancer-free more than a year on, prompting hopes of a potential cure.
Doctors treating one-year-old Layla for leukaemia had warned her parents she had run out of options after chemotherapy and a bone marrow transplant failed to halt the aggressive disease.
But a ground-breaking technique allowed scientists to create designer immune cells to help her own body to fight back, and 20 months later she is still healthy and leukaemia-free.
Experts hope that Layla, now two, will prove to be the first person in the world to be saved by the gene editing technique.
Those behind her treatment at Great Ormond Street Hospital (GOSH) in London now hope the breakthrough could pave the way for future cures for other diseases.
It comes after scientists announced last week that techniques to edit human genetic code could cure all inherited diseases within a generation, with two major US research institutions recommending that gene editing of human eggs, sperm and embryos should be allowed in medical research.
Layla was diagnosed with acute lymphoblastic leukaemia – the most common form of cancer in children – when she was just 14 weeks old.
Doctors described her case as ‘one of the most aggressive we have ever seen’ and began chemotherapy, but both it and a subsequent bone marrow transplant failed.
Her parents were warned she was dying, but GOSH consultants began working with scientists from University College London to try the experimental gene therapy.
It had only been trialled on mice, but Layla’s family was adamant doctors should try the treatment, and the team received special approval to use it on a human patient for the first time.
They took immune system cells, known as T-cells, from a healthy donor and added new genes to them to help them seek out and destroy the leukaemia.
Unlike conventional gene therapy, they also used molecular ‘scissors’ to snip away bits of the T-cells’ DNA that would have attacked Layla’s other, healthy cells.
Gene editing also meant they could strip out elements which would have caused Layla’s body to reject the donor cells.
Just weeks after she was given a single 1ml infusion of the edited T-cells, doctors saw test results that showed the treatment was working.
Now, 20 months after the procedure, tests have shown no sign of the leukaemia. The treatment has since been used on a 15-month-old girl with the same form of cancer, who is now in recovery.
Layla’s mother Lisa told the Sunday Times: ‘We were so worried that it wouldn’t work and when the doctors told us her cancer had gone we couldn’t believe it.
‘We’re so grateful to all the doctors and nurses at GOSH for everything they’ve done for us. We wish we could give them a Nobel prize.’
Waseem Qasim, a professor of cell and gene therapy at UCL and a consultant immunologist at GOSH, said the T-cell treatment was still undergoing trials, but could be used in the future against other blood cancers in adults and children.