Reply To:
Name - Reply Comment
Last Updated : 2024-04-19 16:08:00
 The female Aedes Aegypti mosquito, with characteristic black and white stripes or spots on its body, is responsible for transmitting the terrible Dengue virus. It is also called the break-bone fever due to the abdominal bone and muscle pain that occurs sometimes. Annually, there are an estimated 390 million cases of which 25,000 are fatal.
The female Aedes Aegypti mosquito, with characteristic black and white stripes or spots on its body, is responsible for transmitting the terrible Dengue virus. It is also called the break-bone fever due to the abdominal bone and muscle pain that occurs sometimes. Annually, there are an estimated 390 million cases of which 25,000 are fatal.
Dengue originated some 800 years ago amongst monkeys and was subsequently transmitted to humans. The virus was restricted to Africa and Southeast Asia until the mid-20th century when it began to spread globally. Latin American countries such as Brazil, Colombia and Venezuela have reported the greatest number of cases.
A significantly-higher number (above 50,000) of Dengue cases have been reported in Sri Lanka since 2016. Around 30% of Dengue patients in 2017 were children. There were 34,765 cases reported in Sri Lanka from January to July 2019, a 4.42% increase compared with the same period in 2018. Sri Lanka needs to take immediate and effective measures to control this deadly mosquito-borne malady. It is our duty to ensure the protection of people before the untimed languishing of the future generation.
In 2017, Sri Lanka suffered an outbreak of Dengue that took 320 lives, with 186,101 cases having been reported. According to the WHO, it was significantly higher than the average number of cases reported since 2010. It can be seen from Figure 01 that there was an increase in cases reported in June-July and December-January.
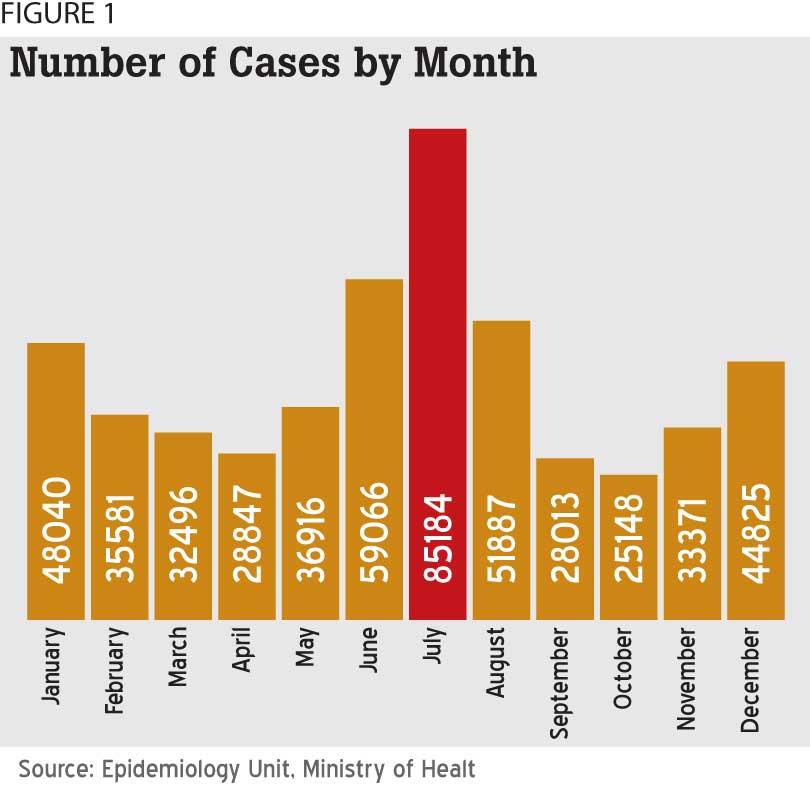
Aedes Aegypti mosquitoes lay eggs in stagnant water. The positive relationship with monthly rainfall and cases of Dengue has been conducive in spreading the virus after the rainy season. Usually, Dengue cases are reported considerably after the inter-monsoon period following the North-East monsoon (March to April) and the inter-monsoon period following the South-West monsoon (October to November). The Western Province is the most threatened by Dengue. The most prevalent cases by districts for the year 2018 were Colombo (10258), Gampaha (5857), Batticaloa (4843), Jaffna (4058), Kandy (3832) and Kalutara (3155), having the highest reported number of cases.
Studies have shown that the cost of Dengue in Colombo district hospitals in 2012 was Rs.325.6 million with an average cost of Rs.113,379.13 per patient. The study found that the average cost of managing a paediatric patient with DHF was Rs.79,656.40 (Health System Cost, 2012) based on data from the Colombo District. In particular, Divisional Secretariats including Dehiwala-Mt. Lavinia, Moratuwa, Kolonnawa, Nugegoda, Maharagama, Kesbewa, Kaduwela, Homagama, Padukka and Hanwella (all under the administration of Regional Directorate of Health) and Colombo and Thimbirigasyaya (both under the Health Department of CMC) were accounted for by this study. When calculating the costs of Dengue, relevant fixed and variable cost elements are taken into consideration including drugs and supplies, utility and maintenance, human resource and other subsidiary cost elements. This can be seen in Figure 02.
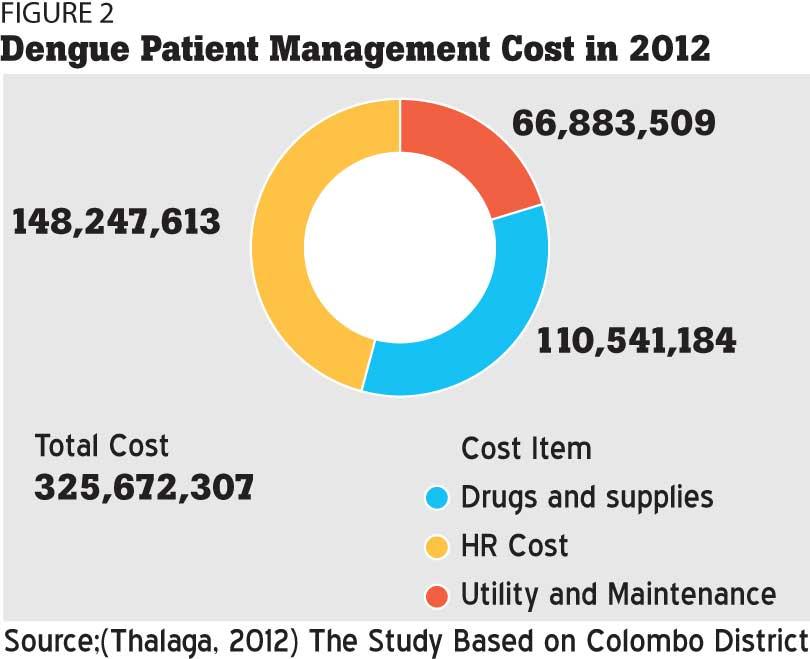
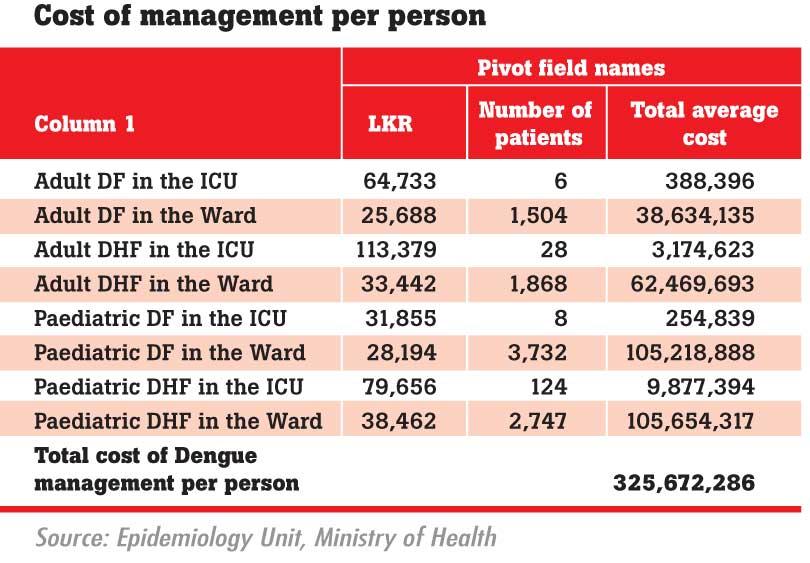
Chart 01 explains the financial cost of managing paediatric and adult patients who suffered from Dengue or Dengue hemorrhagic fever. According to data provided by the Health Ministry, an average of Rs.60,048.56 was spent on a pediatric patient who suffered from Dengue fever and Rs.118,118.10 on Dengue hemorrhagic patients. An average of Rs.90,420.26 is allocated for adult patients who suffered from Dengue and Rs. 146,821.43 for Dengue hemorrhagic patients.
Chart 01
In addition to these visible cost elements, the roots of the financial burden of Dengue go much deeper. A study was conducted at Lady Ridgeway Hospital to investigate the external financial expenditure of break-bone fever. The study focused on analysing both expenses for the hospital as well as external costs for households. The study was conducted from December 1, 2012, to May 31, 2013, including three months of high disease incidence and three months of low incidence. 507 child patients aged up to 12 years were admitted to two wards and 137 observants who fulfilled the requirements were taken into consideration.
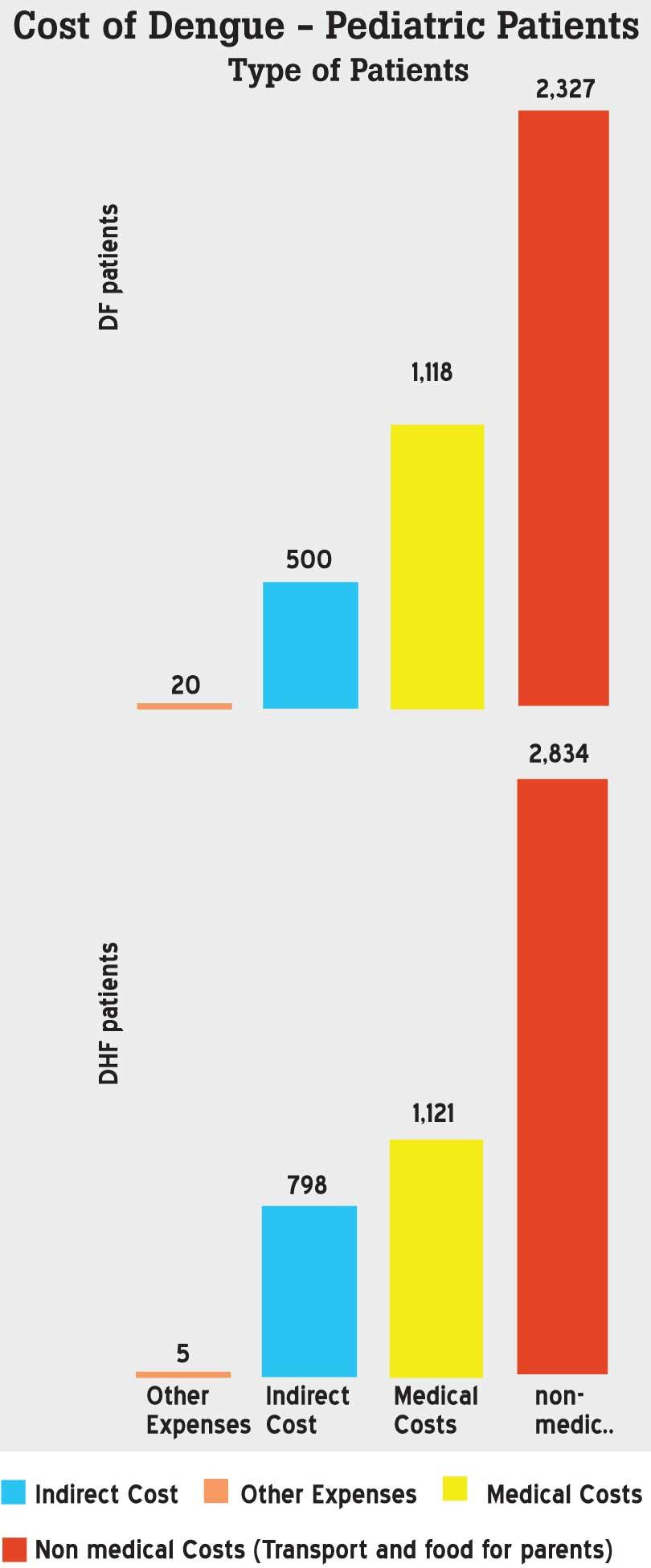
As illustrated by Figure 03, the total financial burden for the households of patients suffering from Dengue fever is Rs.3,965 and Rs.4,758 for Dengue hemorrhagic patients per illness episode. Food for parents, cost of transportation and lodging are considered under non-medical costs and further investigation and cost of purchasing medicine are included in medical costs. A major element of indirect cost is the loss of working hours. Loss of work is not applicable in this study as all patients are below 12 years. But the loss of income to the household due to unpaid leave taken by parents has been considered as an indirect cost.
Figure 03
It is evident that Dengue has put a huge financial constraint on households. The poverty line of Sri Lanka is Rs.1,423, and 6.7% of the population live below the national poverty line, according to the Asian Development Bank. That implies the cost of treating Dengue (non-hemorrhagic) fever is 278.64% greater than the poverty line.
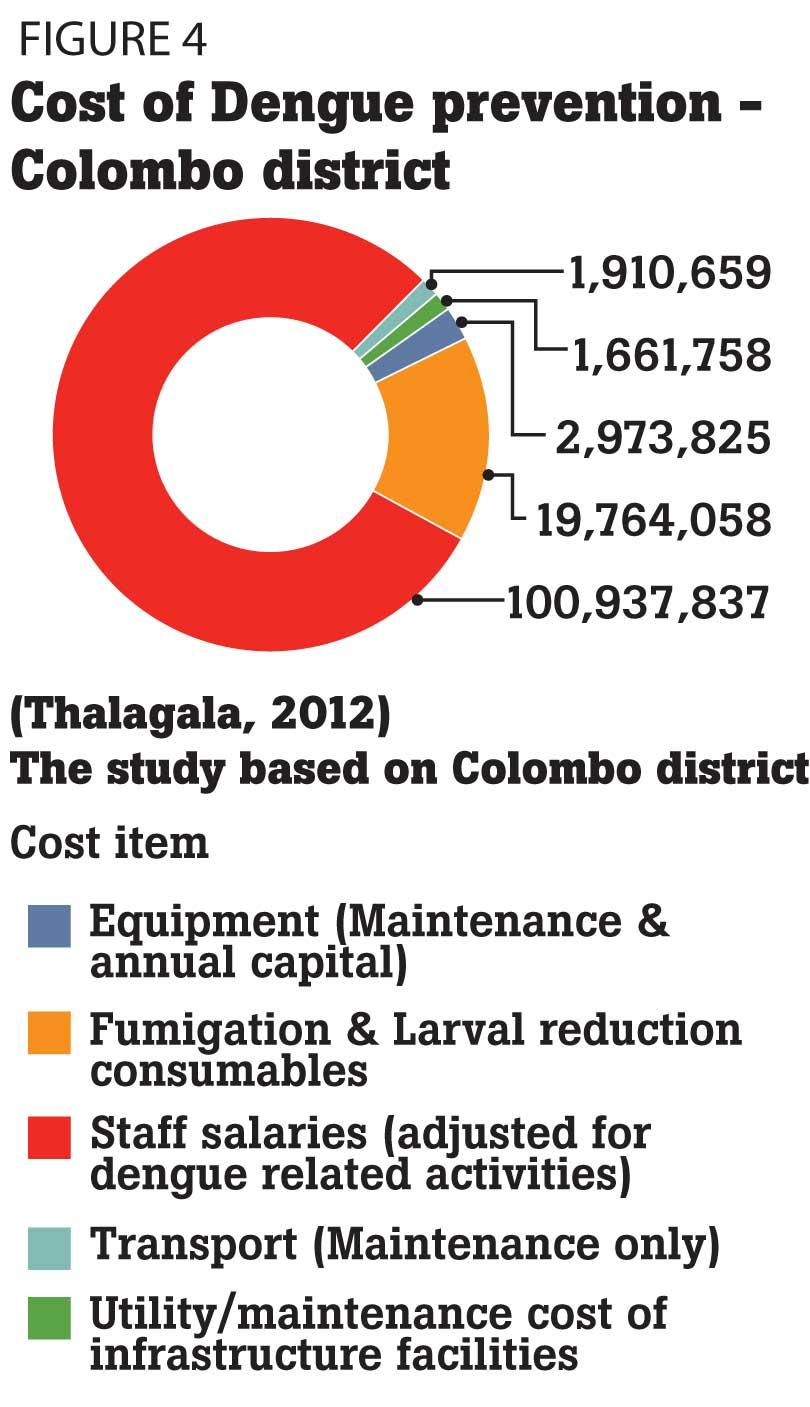
Most of the affected countries have focused on the prevention of Dengue. Figure 04 shows the cost of Dengue prevention programmes implemented in the Colombo District. Fumigation consumables including kerosene oil, diesel, petrol, insecticides and larval reduction consumables including abate granules and liquids, BTI local and bativec liquids have been taken into account. The required machines, vehicles, infrastructure and other relevant elements were also considered. In Sri Lanka, the emphasis is on fumigation and raising awareness.
In other countries, communities seem to be much more aware of Dengue prevention and elimination. They have implemented advanced and innovative projects to control the virus physically, biologically and chemically. A successful biological project has been tested in many countries including Townsville-Australia, Panama, Brazil, Colombia, Indonesia and Vietnam. They have released captive-bred male mosquitoes with a naturally occurring bacteria called “Wolbachia” to mate with local mosquitoes. The bacteria hinder Dengue transmission and today, researchers of Monash University believe that the same method can be used to control “Zika” and “Malaria.”
The project cost 15 Australian Dollars per person in Townsville. In Lahore, Pakistan, a mobile application called ‘Clean Lahore’ was created as a response to the rapid spread of the virus. The general public can make complaints on uncleanness and improper waste collection through the application with live pictures, live GPS location and comments. This proved to be very successful in reducing the number of cases. In Brazil, the Vector Species Genetic Modification method was tested and resulted in an 85% decline in the Aedes Aegypti population. This method works by releasing genetically-modified vector species of mosquitoes to the environment.
All countries are trying their best to reduce the spread of the virus in order to protect human lives from Dengue. According to the research conducted based on the Colombo District, the estimated per capita cost of Dengue prevention and control in Colombo was Rs.55.10 (USD 0.43) in 2012. It is just USD 0.03 per person monthly which lags behind USD 0.13 per month in Panamaand USD 1.88 per month in Cuba. It is clear that Sri Lanka could do more to allocate funds to implement projects that can curb the spread of the malady.

Add comment
Comments will be edited (grammar, spelling and slang) and authorized at the discretion of Daily Mirror online. The website also has the right not to publish selected comments.
Reply To:
Name - Reply Comment
On March 26, a couple arriving from Thailand was arrested with 88 live animal
According to villagers from Naula-Moragolla out of 105 families 80 can afford
Is the situation in Sri Lanka so grim that locals harbour hope that they coul
A recent post on social media revealed that three purple-faced langurs near t