Reply To:
Name - Reply Comment
Last Updated : 2024-04-25 21:49:00
We may need a lot of patience to live a new-normal as one single strategy might not be fully effective in the long run
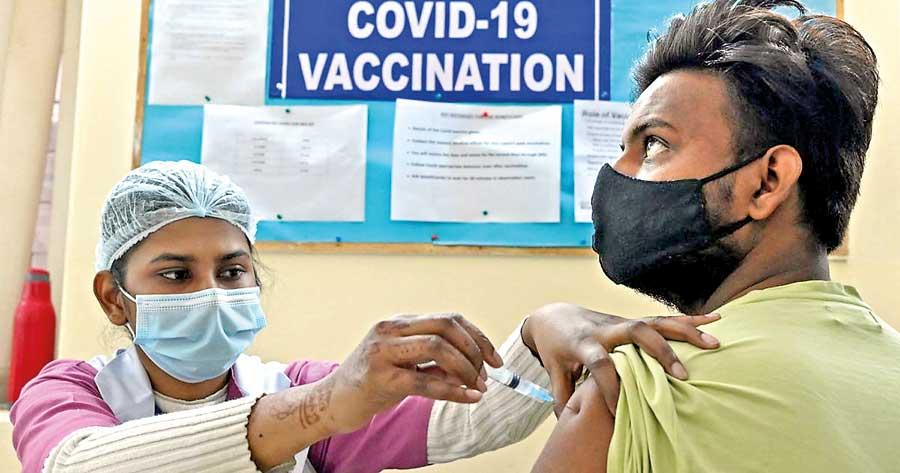
SARS CoV-2 is a well-adopted human respiratory virus to bully the human community globally. It is useful to compare this virus with a few other viruses of similar public health importance.
compare this virus with a few other viruses of similar public health importance.
The previous virus, SARS CoV-1 was highly infectious only several days after the beginning of the symptoms in a patient, therefore transmission was mainly linked to symptomatic cases. Because of that, it was not difficult to break the chain of transmission as the patients were mainly in hospitals when they were highly infectious.
In comparison, SARS CoV-2 is highly infectious right on the day of the first symptoms and on the first two days pending to develop symptoms. In addition, asymptomatic infected people are significantly contributing to the transmission as well. Further, most people are significantly infectious during the first week after the initial establishment of infection.
This pattern of transmission is rather unique to SARS CoV-2 and that is why it is more transmissible than seasonal Influenza viruses as well.
In this background of transmission, the emergence of SARS CoV-2 variants poses added challenge by its ability to achieve much higher transmission rates, high complication rates and some ability to escape the vaccine-induced protection as well. And, these variants can emerge as a result of few simple mutations in the virus gene.
The currently used injectable vaccines do not seem to significantly interrupt the transmission of this virus (other than variable individual protection) with the emergence of new variants.
Therefore, primary vaccination alone may not be sufficient to face the future challenges of this changing virus. In this context, it is essential to block the transmission of the virus using other proven measures (social distancing, movement restriction, appropriate mask, hand hygiene and prevention of overcrowding -especially in indoor settings) in parallel to the injectable vaccination programmes.
In the 1960s, injectable polio vaccines provided individual protection but it was the oral polio vaccine that could block polio community transmission because it could add protection at the entry point of the virus (mouth).
Similarly in the future, it might be possible for an effective SARS CoV-2 nasal spray vaccine to establish protection at the entry points (nose and mouth) to reduce the transmission rate more effectively in comparison to injectable vaccines. We have to wait and see about that option.
Seasonal influenza viruses have been in the global community for decades with a seasonal pattern of infection. Its transmission rate is low compared to SARS CoV-2 and morbidity and mortality risks are mainly only in defined risk groups and the rates are also low compared to SARS CoV-2.
It is unlikely to have complications or fatalities outside the identified risk groups with seasonal influenza. Also, seasonal influenza vaccines are recommended annually only for high-risk groups.
The transmission of the influenza virus is affected by climate and weather conditions. Therefore, transmission can be naturally prevented, ending the existing outbreaks. If SARS CoV-2 happens to take the place of ongoing community transmission replacing the seasonal influenza viruses, consequences might be very severe as SARS CoV-2 will not act only seasonally but might give rise to a continuous transmission pattern without giving in-between natural breaks like in the case of influenza.
In addition, new variants of SARS CoV-2 might give rise to unpredictable complications in people outside the identified risks groups. In this background, if annual SARS CoV-2 vaccination (with variant adjusted vaccines) is also going to be recommended in future to face the challenge of emerging variants, the impact on health care systems would be enormous. It would be far more difficult than the encounter with the seasonal influenza virus.
Some say that the virus’s ability for giving rise to a number of new variants affecting the outcome of diagnostic, vaccines and therapeutics would be limited. It may be relieving speculation. But we can never underestimate viruses’ potential to unexpectedly surprise humans with evolving problems related to genetic changes. Therefore, it might be difficult to predict the future outcome of the encounter between the human body and this changing virus.
This virus is the potential to torment the human population globally for a long period with its potential to create evolving situations making us exhausted. And also, there is no single perfect-zero-risk method to manage this pandemic.
It would be a trial-and-error process that should progress based on accumulating scientific data and its future projections. When we try to look for a zero-risk method (when it doesn’t exist), the outcome will be missing priorities, wasting resources for minor risks leaving out gaps in major risks leading to pandemic fatigue.
Therefore, it is essential to scientifically and technically categorize the risks in an ongoing review to allocate resources rationally to negotiate major risks. We need to run a marathon here not a sprint (sustainability of efforts is more important for ongoing long-term efficacy).
In managing this pandemic, several strategies are used parallelly such as testing, quarantine, isolation, treatment, prevention, movement restriction and vaccination. There are three important aspects in the implementation of these strategies about the management of this pandemic;
Defining our specific objectives (targets) in managing this pandemic long-term considering both feasibilities and a safe margin of error to manage limited resources (focussing both on the sustainability of strategies and prevention of pandemic fatigue)All strategies should be synchronized and interplayed mutually to achieve the timelines of defined objectives (testing, quarantine, isolation, prevention and vaccination strategies should be mutually compatible with one another to give out a cost-effective and sustainable outcome)All strategies should be implemented in a way that the local data could be generated for ongoing situation analysis and timely policy decision making
Although it is simple to describe the above measures, it will be a challenging task to implement them practically. More hands with high technical capacities are needed in a sound operational mechanism of coordination to do an ongoing analysis of global and local COVID data to make timely policy decisions with future projections.
This is a global crisis and every country is struggling to control the pandemic in a sustainable way preventing both pandemic fatigue and economic instability. Management of this crisis cannot be done in one single perfect way. Every measure has its pros and cons. It would be a good moral approach to highly appreciate our achievements so far as a country while proactively projecting for the future with learnt lessons on a scientific basis.
As a society, we may need a lot of patience to live a new normal state of living as one single strategy (testing or vaccination) might not be fully effective in the long run. Basic prevention measures, social distance, movement restriction, appropriate mask, hand hygiene and prevention of overcrowding especially in indoor settings would be the trump cards even at the beginning of this COVID vaccination era.
The author Dr Nadeeka Janage is Consultant Medical Virologist at the Medical Research Institute.

Add comment
Comments will be edited (grammar, spelling and slang) and authorized at the discretion of Daily Mirror online. The website also has the right not to publish selected comments.
Reply To:
Name - Reply Comment
US authorities are currently reviewing the manifest of every cargo aboard MV
On March 26, a couple arriving from Thailand was arrested with 88 live animal
According to villagers from Naula-Moragolla out of 105 families 80 can afford
Is the situation in Sri Lanka so grim that locals harbour hope that they coul