Kidney transplantation is the optimum treatment for end-stage kidney failure. Although the preparation and progress to a kidney transplant involves a complex series of events, the end result is a normal functioning kidney and a new lease of life.
What they do
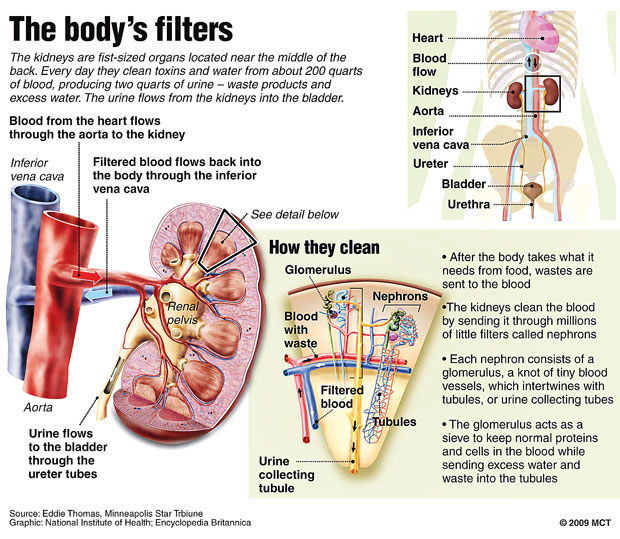
Kidneys are essential for life. Humans usually have two kidneys placed in the retroperitoneum (behind the intestines) which are involved in numerous essential functions which include:
- clearance of toxins from the body via urine
- maintaining water balance
- contributing to the control of
blood pressure
- production of certain hormones etc.
What causes kidneys to fail?
There are two types of kidney failure; acute (sudden and often reversible) and chronic (long-standing and often irreversible).
Acute kidney failure is often caused by conditions such as infections, use of toxic drugs and severe dehydration. It starts suddenly and progresses rapidly. However, with early identification and proper treatment, this condition is often completely reversible. Chronic kidney failure has a slower progression often causing gradual deterioration of the kidneys over several years. The commonest reasons for chronic kidney
failure are:
- diabetes
- hypertension
- kidney stones and repeated infections
- long-term use of toxic medications
- immunological diseases (where the body starts producing antibodies that harm one’s own kidneys) etc.
What is end-stage kidney failure?
Chronic kidney failure progresses slowly. In the initial stages, it can be controlled with medication. End-stage kidney failure is when chronic kidney failure has progressed to the extreme to cause complete kidney failure where medical treatment is inadequate.
End-stage kidney failure requires renal replacement therapy. Renal replacement therapy is where the functions of the kidneys are performed artificially by way of dialysis or transplantation of a new kidney.
Renal transplantation is the best long-term treatment for end-stage kidney failure which gives the longest chance of survival and best quality of life.
Transplant
Donor kidneys can be from live donors or deceased (dead) donors. Live donor kidneys give the best outcomes by way of long term survival. Donating a single kidney is perfectly safe for a healthy person. However, live donors are not always easy to find. The alternative is a deceased donor. These are patients who suffer from ‘brain death’ in hospitals following accidents, strokes etc.
How to select a suitable kidney?
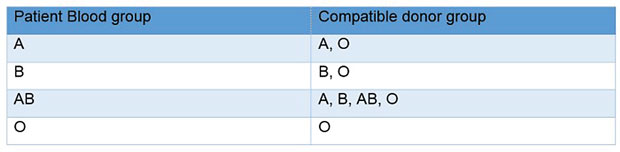
The first thing is to make sure that the potential donor is compatible with the recipient. There are two types of compatibility tests carried out in hospital.
The first basic compatibility is for the
blood group.
The second stage of compatibility testing is for tissue antigens called Human Leucocyte Antigens (HLA) and crossmatch. The HLA matching will determine the exact compatibility of the donor and the recipient. The better the match, better the outcome!
Can anyone be a donor?
Voluntary living donors are extensively checked and screened prior to a transplant. A potential donor should be completely healthy without any evidence of on-going disease.
Under the Sri Lankan law, all male donors should be over 25 years of age and all female donors should be over 30 years of age although this may be subject to individual consideration in exceptional cases such as a parent donating to a child.
Can anyone have a transplant?
Almost anyone can have a transplant. Before the intended transplant, the hospital will carry out specific tests to determine fitness for surgery. This will include a few tests including a chest X-ray, ECG and Echocardiogram to determine the fitness of the heart.
Legal aspects
A potential donor and recipient will initially face an ethical committee examination.
Then the donor’s and patient’s reports are submitted to the Ministry of Health where an independent inquiry into the transplant is conducted to ensure the necessary legal documents are in place. Next, the Director General of Health Services in the Ministry of Health will formally authorize the transplant.
Individual authorization from the Ministry of Health for each transplant is a pre-requisite. Once those authorization documents are received by the hospital, the medical team will finalize the date for the transplant.
Admittance
The majority of patients for transplants are admitted to the hospital either the day before or the morning of the transplant. Some basic tests are repeated and the patient will have a preliminary dialysis before the transplant.
After admission
To ensure the patient is ready for the operation, several things will be done. Hair on the chest and abdomen will be shaved. The patient also undergoes a bath with antiseptic soap/solution before the operation.
The surgery will be carried out under general anaesthesia. Therefore, the patient will fast for approximately 6 hours before the operation.
Process
The transplant is performed in the operating theatre. In a live donor transplant, both the donor and the patient will be operated on at the same time. In the instance of a deceased donor transplant, the donor kidney may be brought from the same or a different hospital.
The new kidney is placed in the lower abdomen usually on the right side.
During the transplant, the patient will have a catheter inserted to his/her bladder. This catheter will allow urine to be collected without the patient having to get up and empty the bladder.
Duration
The transplant operation generally takes approximately 3-4 hours. However, in rare instances, where there is some complexity, the operation may be prolonged.
After surgery
After the surgery, the patient will be taken to the intensive care unit. The patient will usually remain in the ICU for 24-48 hours.
Basic precautions
- Limit the number of visitors
- Always wear a face mask
- Avoid infection transmission – use of antiseptics, hand washing, face mask
- Eat home cooked meals
- Take all medications given by the hospital
- Visit the medical team as advised
 Kidney transplantation is the optimum treatment for end-stage kidney failure. Although the preparation and progress to a kidney transplant involves a complex series of events, the end result is a normal functioning kidney and a new lease of life.
Kidney transplantation is the optimum treatment for end-stage kidney failure. Although the preparation and progress to a kidney transplant involves a complex series of events, the end result is a normal functioning kidney and a new lease of life.