Reply To:
Name - Reply Comment
Last Updated : 2024-04-19 22:36:00
Non-alcoholic fatty liver is a condition, where fat is accumulated in the liver of people, who drink little or no alcohol.
“This a common condition, especially in the South East Asian countries where 30-40 percent of the population
is affected,” explains Consultant Gastroenterologist, Dr. Ranjith Peiris.
“What is tricky and dangerous about the disease is that it shows no symptoms until it progresses to a very advanced stage, resulting even in liver failure,” he warned.
The increasing prevalence of non-alcoholic fatty liver is predicted to become the most common cause of advanced liver disease in the world in the coming decades.
In an interview with the Daily Mirror , Dr. Peiris explains how the condition can be prevented.
Q Why is the Asian population more prone to this condition?
The situation could be largely attributed to the epidemic of diabetes in this region, especially in the South Asian region. Coupled with this, lack of exercise, fast-food and obesity, which are all results of urbanization, have contributed to this situation. South Asians may also have a genetic predisposition to store more fat in the abdominal cavity and in the liver.
Q Who are at the risk of developing non-alcoholic fatty liver?
Diabetes is a leading pre-disposing factor. There are two types of diabetes: Type 1 diabetes and Type 2 diabetes. Type 2 diabetes, onset of which is at maturity (Occurring later in life unlike Type 1 diabetes which can be contacted in early life) could trigger fatty liver.
Non-alcoholic fatty liver is prevalent in 50 percent of the diabetics. Overweight and obese people are also at risk, high cholesterol (Those with high triglycerides). Those who lead sedentary lifestyles, those who consume oily food and fast food are also at risk.
If anyone has the above mentioned high risk factors, we encourage him or her to do a liver profile (Which is a blood test) at least every six months and an ultra sound scan of the abdomen at least  once a year.
once a year.
Fatty liver can also be prevented by cutting down on the intake of fast food/oily food and red meats. High fibre products such as vegetables and green leaves and fish will help reducing obesity reducing incidence of fatty liver.
Q Is there a genetic involvement in developing the condition?
We presume a genetic predisposition as diabetes, which is a risk factor that has a genetic involvement. However, worldwide research is still underway to discover the genetic factor. Similar to diabetes, most cases are expected to be due to the influence of multiple genes, so a single genetic factor is unlikely.
Q Are both males and females equally susceptible?
Yes, both genders are equally susceptible.
Q Are there symptoms of this condition?
This is what is tricky about this disease as it has no symptoms and some may experience a mild pain in the right side of the abdomen if the condition has advanced.
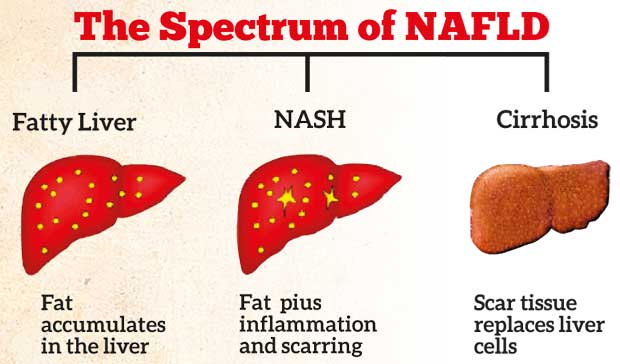
Non-alcoholic fatty liver entails a spectrum. The very early stages are known as steatosis, where there is excess fat in the liver. This could progress into the second stage known as steato-hepatitis. This phase could progress into cirrhosis and also other complications including liver cancer and finally liver failure.
Q In the absence of symptoms, how is fatty liver diagnosed?
In about 80 percent of cases, fatty liver is diagnosed when patients are tested for some other condition/disease. Unfortunately, some patients present with advanced cirrhosis of the liver, with no  other apparent cause (cryptogenic cirrhosis).
other apparent cause (cryptogenic cirrhosis).
Q What are the diagnostic tools/tests used?
A lipid profile which is a blood test is the preliminary test done. Ultra sound scan of the abdomen, results of which are given in three gradings:
Grade 1 would indicate early stages of the condition followed by Grade 2 which is the more advanced stage and Grade 3, which is the most complicated stage.
If the diagnosis is uncertain and there are doubts, we do a liver biopsy. However, there are other causes that may give similar tests results (e.g: Viral Hepatitis) and these may need to be excluded by blood tests.
Q What are the repercussions of mismanaged non-alcoholic fatty liver?
Generally, 20 percent of mismanaged cases with steato-hepatitis would end up in cirrhosis. If the condition is mismanaged it could lead to liver cancer as well. This is why irrespective of the age, high risk groups (those with risk factors) are advised to do a liver profile every six months and an ultra sound scan of the abdomen annually to detect non-alcoholic fatty liver very early. Even those in their early 20s could get non-alcoholic fatty liver, if they have risk factors which we discussed earlier.
Q How is the condition treated?
At the initial stage (steatosis) without any clinical intervention, the situation could be managed by modifying the risk factors. Weight-loss is the most effective method to improve it, and a target of 3-5% of the body weight loss is recommended. If the condition has advanced, we treat it with a combination of drugs and modification of risk factors.
Risk factors like diabetes and high cholesterol levels need to be managed carefully. There is no single drug proven to be effective in curing fatty liver, but extensive research is currently underway worldwide to discover new agents. There is no place for surgery in fatty liver. One should remember that sometimes medication could be life-long depending on the severity of the condition. Proper monitoring of the condition without resorting to ad hoc treatment is imperative.

Add comment
Comments will be edited (grammar, spelling and slang) and authorized at the discretion of Daily Mirror online. The website also has the right not to publish selected comments.
Reply To:
Name - Reply Comment
On March 26, a couple arriving from Thailand was arrested with 88 live animal
According to villagers from Naula-Moragolla out of 105 families 80 can afford
Is the situation in Sri Lanka so grim that locals harbour hope that they coul
A recent post on social media revealed that three purple-faced langurs near t