Reply To:
Name - Reply Comment
Last Updated : 2024-04-19 00:03:00
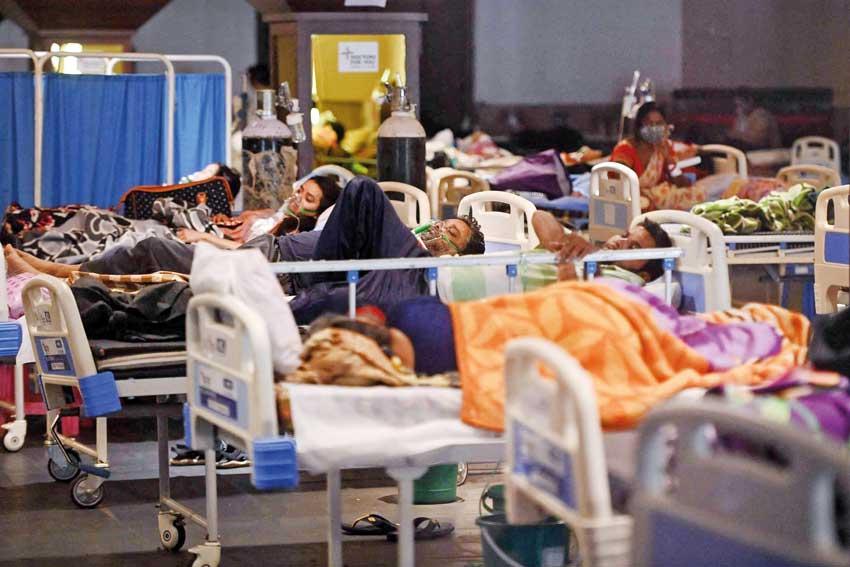
 COVID-19 may cause lung complications such as pneumonia and in the most severe cases COVID-19 patients might lose the ability to breathe normally. This is known as respiratory failure that results from severe inflammation in the lungs. Inflammation arises when there is damage to cells and in the case of COVID-19 it infects lung cells and damages them. Inflammation causes swelling, which is the result of increased fluid moving to the site of injury or damage. Unfortunately, when fluid moves into the lungs the lungs cannot perform their normal function; taking in oxygen and releasing carbon dioxide. To enlighten you on the topic we spoke to Dr. Sujeewa Weerasinghe, National Organizer of the Chartered Society of Physiotherapists, Vice President of the World Disability and Rehabilitation Professionals Association who also possess an International
COVID-19 may cause lung complications such as pneumonia and in the most severe cases COVID-19 patients might lose the ability to breathe normally. This is known as respiratory failure that results from severe inflammation in the lungs. Inflammation arises when there is damage to cells and in the case of COVID-19 it infects lung cells and damages them. Inflammation causes swelling, which is the result of increased fluid moving to the site of injury or damage. Unfortunately, when fluid moves into the lungs the lungs cannot perform their normal function; taking in oxygen and releasing carbon dioxide. To enlighten you on the topic we spoke to Dr. Sujeewa Weerasinghe, National Organizer of the Chartered Society of Physiotherapists, Vice President of the World Disability and Rehabilitation Professionals Association who also possess an International
Certificate in Coronavirus.
The pneumonia that COVID-19 causes tends to affect both lungs. The air sacs in the lungs fill with fluid, limiting their ability to take in oxygen and this causes shortness of breath, cough and other symptoms.
While most people recover from pneumonia without any lasting lung damage. The pneumonia associated with COVID-19 can be severe. Even after the disease has passed, lung injury may result in breathing difficulties that might take months to improve.
Another possible complication of a severe case of COVID-19 is sepsis. Sepsis occurs when an infection reaches and spreads through the bloodstream, causing tissue damage everywhere it was present. Lungs, heart and other body systems work together. During sepsis the cooperation between the organs falls apart. The entire organ system can start to shut down, one after another, including the lungs and heart.Sepsis, even when survived, can leave a patient with lasting damage to the lungs and other organs.
Boosting immunity 
Staying well fed is important for overall health. Proper hydration maintains proper blood volume and healthy mucous membranes in the respiratory system, which can help them better resist infection and tissue damage.
Physiotherapy input to the prevention and treatment of ICU acquired weakness is vitally important, but COVID-19 brings unique challenges and some adaptations to the way that care is delivered. ICU physiotherapy, mechanical ventilation, respiratory management, physical function, outcome measurement and long-term outcomes after critical illness are relevant when patients are hospitalized for COVID-19 cases. After an illness like COVID-19, it may take your body some time to feel normal again.
Breathing is extremely beneficial for the lungs, boosting lung capacity. It is very important for the mind to be calm because when we are stressed or anxious, breathing is affected and the respiratory rate goes up. This puts pressure on the lungs.Breathing techniques or exercises are being recommended to help people get air right into the bases of their lungs if they are suffering from COVID-19. The breathing techniques won’t cure COVID-19, but they may help to alleviate some of the respiratory symptoms by helping to clear mucus or secretions from the lungs. Shortness of breath, or dyspnea, is a common respiratory symptom associated with COVID-19.
 Deep breathing can also be helpful for mind and body and meditation and relaxation. Just the act of concentrating on your breathing may release some stress and make your feel good. Deep breathing can help restore diaphragm function and increase lung capacity. The goal is to build up the ability to breathe deeply during any activity, not just while at rest. Deep breathing exercises can also lessen feelings of anxiety and stress, which are common for someone who experienced severe symptoms or was admitted to a hospital. Sleep quality may also improve with these breathing exercises.
Deep breathing can also be helpful for mind and body and meditation and relaxation. Just the act of concentrating on your breathing may release some stress and make your feel good. Deep breathing can help restore diaphragm function and increase lung capacity. The goal is to build up the ability to breathe deeply during any activity, not just while at rest. Deep breathing exercises can also lessen feelings of anxiety and stress, which are common for someone who experienced severe symptoms or was admitted to a hospital. Sleep quality may also improve with these breathing exercises.
Anyone can benefit from deep breathing techniques, but they play an especially important role in the COVID-19 recovery process. The exercises can be started at home during self-isolation and easily incorporated into your daily routine.

Add comment
Comments will be edited (grammar, spelling and slang) and authorized at the discretion of Daily Mirror online. The website also has the right not to publish selected comments.
Reply To:
Name - Reply Comment
On March 26, a couple arriving from Thailand was arrested with 88 live animal
According to villagers from Naula-Moragolla out of 105 families 80 can afford
Is the situation in Sri Lanka so grim that locals harbour hope that they coul
A recent post on social media revealed that three purple-faced langurs near t

10 Apr 2024
09 Apr 2024