07 May 2021 - {{hitsCtrl.values.hits}}
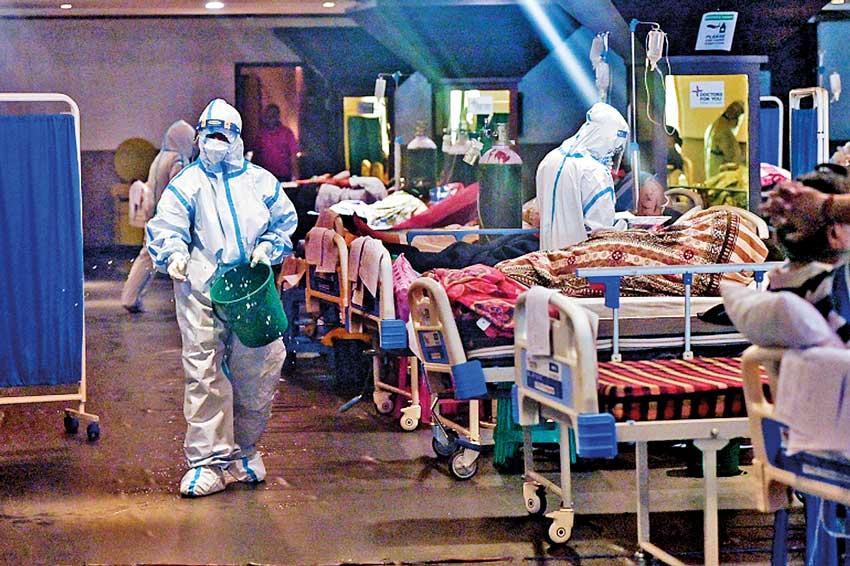
A huge concern lies with regards to the supply of oxygen in managing the latest COVID-19 outbreak. But why do some patients need oxygen therapy and what is the protocol for such therapy?
When does a Covid-19 patient need oxygen support?
A small proportion of Covid-19 patients need oxygen support, when shortness of breath progresses to a more acute condition. Most patients with Covid-19 have a respiratory tract infection, and in the most severe cases their symptoms can include shortness of breath. In a small proportion of such cases, this can progress to a more severe and systemic disease characterised by Acute Respiratory Distress Syndrome (ARDS).
How does Covid-19 trigger shortness of breath?
Shortness of breath occurs because of the way Covid-19 affects the patient’s respiratory system. The lungs enable the body to absorb oxygen from the air and expel carbon dioxide. When a person inhales, the tiny air sacs in the lungs — alveoli — expand to capture this oxygen, which is then transferred to blood vessels and transported through the rest of the body.
In what conditions is oxygen used in Covid-19 clinical management?
According to the clinical management protocol, a person is suffering from moderate disease when he or she is diagnosed with pneumonia with no signs of severe disease; with the presence of clinical features of dyspnea (shortness of breath) and/or hypoxia (when the body is deprived of adequate oxygen supply at the tissue level); fever, cough, including SpO2 (oxygen saturation level) less than 94% (range 90-94%) in room air.
In moderate cases, oxygen therapy is the primary form of treatment: the target is to achieve 92-96% SpO2, or 88-92% in patients with chronic obstructive pulmonary disease. The devices for administering oxygen in moderate disease are nasal prongs, masks, or masks with breathing/non-rebreathing reservoir bags, depending on requirement. The protocol also recommends awake proning (having patients lie on their stomachs) as a rescue therapy to increase oxygenation. Severe cases are defined in three categories: severe pneumonia, acute respiratory distress syndrome, and sepsis. The clinical management protocol recommends oxygen therapy at 5 litres/min. When respiratory distress and/or hypoxemia of the patient cannot be alleviated after receiving standard oxygen therapy, the protocol recommends that high-flow nasal cannula oxygen therapy or non-invasive ventilation can be considered.
“Compared to standard oxygen therapy, High Flow Nasal Cannula Oxygenation (HFNO) reduces the need for intubation. Patients with hypercapnia (exacerbation of obstructive lung disease), hemodynamic instability, multi-organ failure, or abnormal mental status should generally not receive HFNO,” the protocol says.
Source : Indian Express
26 Apr 2024 1 hours ago
26 Apr 2024 1 hours ago
25 Apr 2024 3 hours ago
25 Apr 2024 4 hours ago
25 Apr 2024 4 hours ago