06 Sep 2019 - {{hitsCtrl.values.hits}}
 For a suicidal person, taking his or her life is the only solution to life’s problems. Every year, suicide is among the top 20 leading causes of death globally for people of all ages. It is responsible for over 800,000 deaths, which equates to one suicide every 40 seconds. Every life lost represents someone’s partner, child, parent, friend or colleague. For each suicide approximately 135 people suffer intense grief or are otherwise affected. This amounts to 108 million people per year who are profoundly impacted by suicidal behaviour. Suicidal behaviour includes suicide, and also encompasses suicidal ideation and suicide attempts. For every suicide, 25 people make a suicide attempt and many more have serious thoughts of suicide. But there’s much that could be done in a collective effort. This is why the World Suicide Prevention Day theme which falls on September 10 reads ‘Working together to prevent suicide.’
For a suicidal person, taking his or her life is the only solution to life’s problems. Every year, suicide is among the top 20 leading causes of death globally for people of all ages. It is responsible for over 800,000 deaths, which equates to one suicide every 40 seconds. Every life lost represents someone’s partner, child, parent, friend or colleague. For each suicide approximately 135 people suffer intense grief or are otherwise affected. This amounts to 108 million people per year who are profoundly impacted by suicidal behaviour. Suicidal behaviour includes suicide, and also encompasses suicidal ideation and suicide attempts. For every suicide, 25 people make a suicide attempt and many more have serious thoughts of suicide. But there’s much that could be done in a collective effort. This is why the World Suicide Prevention Day theme which falls on September 10 reads ‘Working together to prevent suicide.’
On that note, the Health Capsule sheds light on the situation in Sri Lanka, what those around a suicidal person should and shouldn’t do and possible interventions.
Working together
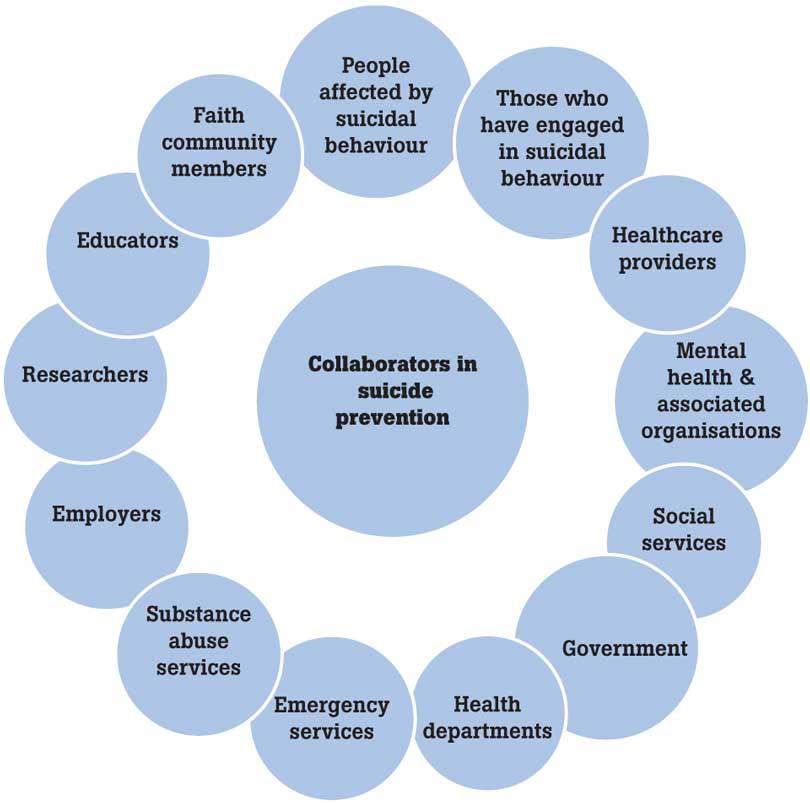
A suicidal person has bottled up his or her emotions. They may see that there’s no way out. In such a situation, just giving an ear to that person is all that is needed. This is why preventing suicide cannot be done single-handedly as it requires the effort of many. It takes family, friends, co-workers, community members, educators, religious leaders, healthcare professionals, political officials and governments. Suicide prevention requires integrative strategies that encompass work at the individual, systems and community level. Research suggests that suicide prevention efforts would be more effective if they span multiple levels and incorporate multiple interventions. This requires the involvement of interventions that occur in communities and involve social and policy reforms, as well as interventions that are delivered directly to individuals.
Suicidal behaviour is universal, knows no boundaries and therefore affects everyone. The millions of people affected each year by suicidal behaviour have exclusive insight and unique voices. Their experiences are invaluable for informing suicide prevention measures and influencing the provision of supports for suicidal people and those around them. The involvement of people with live experience of suicide in research, evaluation and intervention should be central to the work of every organisation addressing suicidal behaviour.
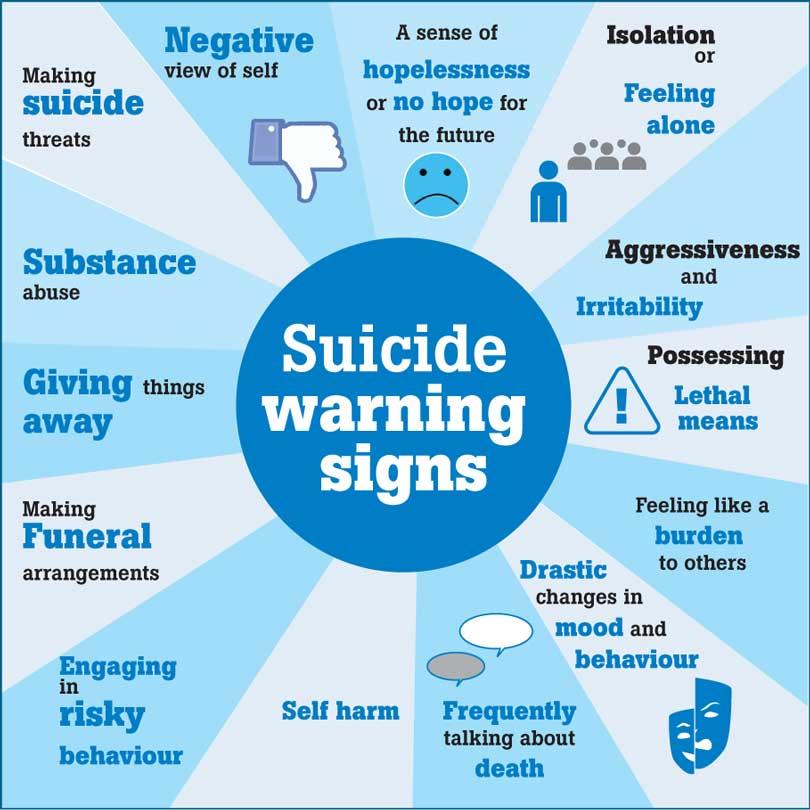
The millions of people affected each year by suicidal behaviour have exclusive insight and unique voices. Their experiences are invaluable for informing suicide prevention measures and influencing the provision of supports for suicidal people and those around them
Listening vs. counselling
“If we take our country we don’t know the exact reason why someone committed suicide mainly due to lack of solid data,” said Dr. Jayamal De Silva, Consultant Psychiatrist at Colombo South Teaching Hospital, Kalubowila and Senior Lecturer in Psychiatry, Faculty of Medical Sciences, University of Sri Jayawardenapura. “More than 50% of people attempt to kill themselves impulsively. This is mainly because of anger, to take revenge or to state a point. They think only about that instance. This is the most common reason. But apart from that a small percentage of people would also have conditions such as depression or a difficult life problem and would need support. But because of the illness they may take their life.”
According to Dr. De Silva, professional counseling is a clinical intervention and expanding on this may not be the best solution for solving problems. “Listening and counseling are different. Those who come for counseling are identified as having depression according to the system. Depression won’t get cured at home. For that they need to seek professional help. They need to be on close watch. But say for example a person is experiencing a stressor such as a disaster, loss of employment or the loss of a loved one, in that instance we are not supposed to force that person to talk.”
What to do and not
When someone is going through a tough time, we often tend to ask them what’s wrong. What we don’t do is give them time to gather their thoughts. But sometimes their changes go unnoticed. According to Dr. De Silva, those around them shouldn’t challenge a person who has thoughts of giving up on life. “Don’t compare their situation with another person’s life. Some people say there are others who have gone through worst situations and such remarks are not going to help this situation. As mentioned earlier, they shouldn’t be forced to talk. What should be done is to make this person realise that most experiences are normal. For example some people get depressed when they fail at an exam. So they could be advised on doing better next time or going for an alternative rather than thinking about the marks.”
“We should also advice the person concerned to keep away from harmful situations such as alcohol abuse or access to sharp objects,” he continued. “On the other hand the patient is also experiencing social withdrawal. They keep bottling-up their emotions which is very unhealthy. Here the patient should be discouraged to continue with what they were planning to do and help them postpone it.”
According to statistics gathered by Sri Lanka Police on the reasons for committing suicide, as many as 350 odd males and around 60 females with chronic diseases and physical disabilities have taken their lives in 2018. “There are also instances when terminally ill patients decide to give up on their lives,” Dr. De Silva added. “Especially in a case like cancer, doctors may say that there’s no hope. So those around the patient could engage in passing time with the patient and ensure that he or she has a dignified departure from the world. These things could be done by people around them.”
BPD is a chronic condition and usually lasts for years. Chronic conditions may lead to more risk of suicide as they don’t tend to recover quickly without treatment
Sumithrayo
 In Sri Lanka, Sumithrayo, a Government-approved charity has been taking the lead in providing confidential emotional support to those who need support. Volunteers are trained to listen to callers who call their hotline on a daily basis seeking support. Here the volunteers give their time to listen rather than telling the other person what to do and not. At rural level, in places where suicides are most prevalent the Organisation deploys trained officers to speak to vulnerable people and families on an individual basis. Volunteers also visit hospitals and befriend patients, provide emotional support for differently-abled people, befriend private sector employees and engage in many other intervention-based approaches.
In Sri Lanka, Sumithrayo, a Government-approved charity has been taking the lead in providing confidential emotional support to those who need support. Volunteers are trained to listen to callers who call their hotline on a daily basis seeking support. Here the volunteers give their time to listen rather than telling the other person what to do and not. At rural level, in places where suicides are most prevalent the Organisation deploys trained officers to speak to vulnerable people and families on an individual basis. Volunteers also visit hospitals and befriend patients, provide emotional support for differently-abled people, befriend private sector employees and engage in many other intervention-based approaches.
Personality disorders
We should also advice the person concerned to keep away from harmful situations such as alcohol abuse or access to sharp objects
25 Apr 2024 57 minute ago
25 Apr 2024 2 hours ago
25 Apr 2024 2 hours ago
25 Apr 2024 3 hours ago
25 Apr 2024 4 hours ago