05 Jul 2019 - {{hitsCtrl.values.hits}}

 Group B Streptococcus (GBS) is one of the main causes of postpartum infection and neonatal sepsis. It mainly concerns pregnant women and requires immediate treatment in order to avoid the adverse effects that are resulted by the infection. Many women around the world have experienced incidents such as preterm labour and child loss at birth. This can be due to inadequate care or the mother’s lack of knowledge on diseases like the GBS infection. Pregnant women should be aware of the diseases that can develop during pregnancy so that they can be safe and keep the baby safe as well.
Group B Streptococcus (GBS) is one of the main causes of postpartum infection and neonatal sepsis. It mainly concerns pregnant women and requires immediate treatment in order to avoid the adverse effects that are resulted by the infection. Many women around the world have experienced incidents such as preterm labour and child loss at birth. This can be due to inadequate care or the mother’s lack of knowledge on diseases like the GBS infection. Pregnant women should be aware of the diseases that can develop during pregnancy so that they can be safe and keep the baby safe as well.
With ‘July’ being the Group B Streptococcus awareness month, the Health Capsule has taken the chance to enlighten Sri Lankan mothers about the GBS infection and its causes and effects.
In order to help raise awareness, Professor Hemantha Dodampahala, Consultant Obstetrician and Gynaecologist, shares his valuable knowledge on this subject.
What is Group B Streptococcus?
This is an infection caused by the bacterium Streptococcus agalactiae, normally found in the intestines, vagina and rectum of all healthy, adult women. This bacteria is generally a harmless commensal bacteria colonizing the gastrointestinal and genitourinary tracts of normal healthy adults. However, it can be dangerous if the microorganism is present in the vagina during labour as it can spread to the baby and cause severe invasive infections.
As Prof. Dodampahala stated it is harmful to both the mother and the baby, but mostly to the baby.
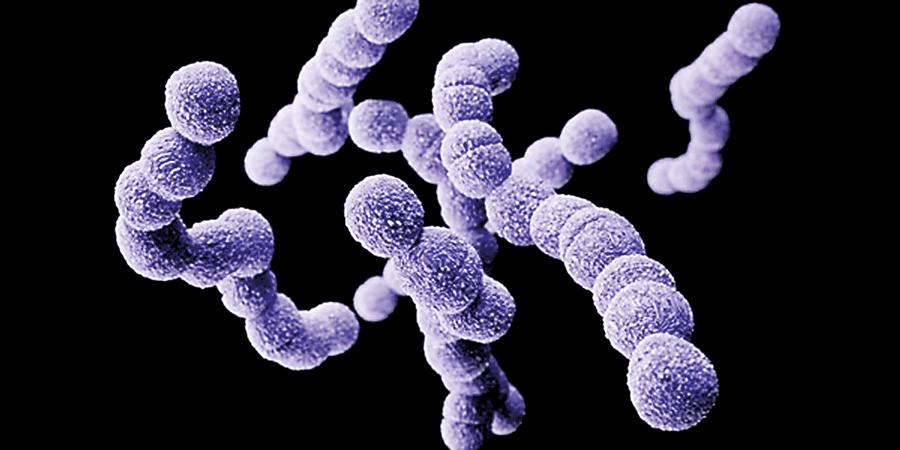
Causes and effects
Prof. Dodampahala provided deep explanation on the causes and effects of the infection. He stated that the main cause is having the infection during labour which will allow it to spread to the baby during vaginal delivery where the baby is exposed to the GBS.
According to him, this perilous disease leads to miscarriage, urinary infection and vaginal discharge. If miscarriage does not occur, it ultimately triggers preterm labour.
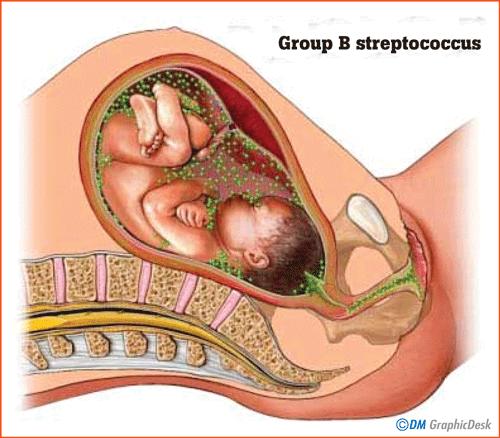
What happens is, the GBS microorganism produces toxins which dissolve the membranes and the water bag starts leaking. Then the bacteria can go and infect the baby. Therefore the major risk is to the newborns.
Since the rupture occurs before the due date, it results in premature birth of the baby. The bacteria enters through the baby’s mouth and spreads into the lungs. This causes severe pneumonia. It can also enter through the nose and affect the brain, causing meningitis. Furthermore, the bacteria can enter the baby’s bloodstream and cause death, which is termed as ‘septicaemia’.
These adverse conditions can also lead to long-term illnesses such as hearing loss, learning problems, cerebral palsy and seizures.
Signs and Symptoms
There are no specific signs seen while the colonized bacteria is carried by the mother. But the infection can develop and the baby will start showing symptoms after birth.
There are two forms of the infection that can take effect on the baby. They are, early-on set and late-on set GBS.
If the form of illness is early-on set GBS, the baby becomes sick and starts showing symptoms such as fever, difficulty-feeding and lethargy within one week after birth.
If the form of illness is late-on set GBS, the baby becomes sick during the first week after birth or a few months later. The complications include fever, difficulty-feeding, lethargy, difficulty in breathing as well as irritability.
Diagnosis
There is no other way than getting a test done in order to identify the presence of the GBS in a pregnant woman.
Prof. Dodampahala stated that the main technique used to diagnose the disease is known as “High Vaginal Swab”. He explained that it is basically done by inserting a cotton swab into the vagina of the patient and getting it into contact with the microorganisms in the upper vagina.
After the sample is obtained, it is sent to be cultured in the laboratory. The results will confirm if the patient is GBS positive or negative.
According to Prof. Dodampahala, this technique is quite convenient and provides 100% accurate diagnosis unlike the other local chemical tests that are available.
The period in which the microorganism can be present is from conception up to delivery. It can appear at any time, especially close to delivery. Therefore, even if tested negative, the mother should continue to be tested from time to time so that it can be detected and diagnosed.
Prevention and Cure
Recognizing the condition as early as possible is very important for the treatment and cure of GBS infection. Treatment should be given as soon as the infection is detected to prevent it from being transmitted to the baby.
Prof. Dodampahala said that antibiotics are the cure to the infection. Penicillin is the main antibiotic given to the patients and it’s given in the form of oral tablets. Other local forms are present but they are not as effective. Bacteria are sensitive to antibiotics and therefore will be destroyed. The full course should be taken to completely wipe out all traces of the GBS. After that, the baby can be safely delivered.
After the baby is delivered, the doctor will examine the baby’s eyes, nose and mouth to ensure that the baby is GBS-free. If the bacteria is found, the baby still needs to be treated.
The baby is the one mostly affected by GBS, leading to many adverse conditions and also death. Therefore, transmission of GBS should be prevented at all costs before things get complicated.
The ‘High Vaginal Swab’ test is a daily routine for pregnant women in foreign countries. But according to Prof. Dodampahala, the test cannot be carried out as a daily routine in Sri Lanka due to the poor availability of facilities.
But in order to avoid such causes, Prof. Dodampahala said that every woman who becomes pregnant should get the test done. Especially, the women who had experienced preterm labour, child loss at birth and those who had given birth to GBS infected babies in their past pregnancies.
This is a serious disease that everyone should be aware of. Regular check-ups and tests should be done by pregnant women to ensure giving birth to a healthy baby.
19 Apr 2024 2 hours ago
18 Apr 2024 4 hours ago
18 Apr 2024 4 hours ago
18 Apr 2024 5 hours ago
18 Apr 2024 6 hours ago