24 Jan 2020 - {{hitsCtrl.values.hits}}
 The World Leprosy Day is observed on the last Sunday of January every year and helps raise awareness about a skin condition that could result in severe deformity if not treated properly. Leprosy can simply be defined as an infection leading to severe nerve damage, deformities, skin infections and sores following the entry of a bacteria known as Mycobacterium leprae into the body. Speaking to Health Capsule, Consultant Community Physician of the Anti Leprosy Campaign of the Ministry of Health, Dr. Kapila Piyasena explained the intricacies of one the ancient diseases that has a history spanning many years. According to Dr. Piyasena, Leprosy was first introduced to Sri Lanka during the Dutch colonial era. The turning point came in 1950s when the World Health Organization introduced a treatment known as Dapson available for leprosy. Ever since, patients suffering with leprosy were treated with Dapson world wide with a gradual decline in the number of cases been reported over the years. However, in 1985 a multi drug therapy was introduced as a much better way of treatment for Leprosy.
The World Leprosy Day is observed on the last Sunday of January every year and helps raise awareness about a skin condition that could result in severe deformity if not treated properly. Leprosy can simply be defined as an infection leading to severe nerve damage, deformities, skin infections and sores following the entry of a bacteria known as Mycobacterium leprae into the body. Speaking to Health Capsule, Consultant Community Physician of the Anti Leprosy Campaign of the Ministry of Health, Dr. Kapila Piyasena explained the intricacies of one the ancient diseases that has a history spanning many years. According to Dr. Piyasena, Leprosy was first introduced to Sri Lanka during the Dutch colonial era. The turning point came in 1950s when the World Health Organization introduced a treatment known as Dapson available for leprosy. Ever since, patients suffering with leprosy were treated with Dapson world wide with a gradual decline in the number of cases been reported over the years. However, in 1985 a multi drug therapy was introduced as a much better way of treatment for Leprosy.
Unlike the various blood tests available to determine the presence of the disease or infection, leprosy is not diagnosed with a blood test
Understanding the disease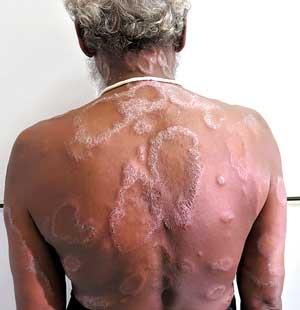
Leprosy initially presents itself as a skin lesion in the form of hypo pigmented patch. While it can occur in any part of the body, people sometimes tend to not take much notice of such skin lesions. One of the peculiar features of this lesion is that in the centre of the patch, one may not feel any sensation compared to the skin around the lesion. Explaining further, Dr. Piyasena said that the lesion is caused by a bacteria known as Mycobacterium leprae , a slow growing bacteria capable of affecting the nerves of the patient.
“The first sign of this is followed by the numbness and tingling sensation of the hands and legs. Eventually this might lead to the total paralysation of the particular nerve. The skin of leprosy patient tends to get burnt resulting in wounds and sores. Due to the lack of flesh in the wounds, infections set in and directly affects the bones. When it affects the bones, it is commonly known as osteomyelitis in the medical world.
In most cases of osteomyelitis, a patient could lose digit by digit of their fingers and toes. This can also damage the eyes. In the case of eyes, it is a well-known fact the eyes are closed when sleeping or blinking and there is a particular nerve known as the facial nerve, which is responsible for this. The facial nerve also gets affected as a result of leprosy, resulting in the inability to close the eyes. When a patient cannot close the eyelids, the eyes get dried up , eventually leading to blindness. Due to loss of toes, one may not even be able to walk if the condition worsens. When the infection affects the cartilage of the patient’s nose, the nose starts eroding, thus causing more facial disfigurement.This is a long process that takes place between 5 to 10 years” the doctor said.
Once the bacteria infects a person, symptoms do not appear at a rapid phase since Mycobacterium leprae is a slow growing bacteria with an incubation period that ranges between 2 years to 20 years. Even if the bacteria is in the body, in most cases one may start observing symptoms only after 10 -15 years. The bacteria usually remains in the nostrils and when the patient carrying the bacteria sneezes or coughs., the bacteria could spread to other individuals through air droplets.
“In public health, we divide leprosy into two sections, namely multibacillary type and paucibacillary type. When there is a large number of bacteria in the body, we call it multibacillary. Comparatively, paucibacillary refers to carrying a less number of bacteria in the body. Multibacillary contains a Lepromatous form of leprosy while paucibacillary contains a Tuberculoid form of leprosy” he said.
Leprosy initially presents itself as a skin lesion in the form of hypo pigmented patch. While it can occur in any part of the body, people sometimes tend to not take much notice of such skin lesions
Diagnosis and treatment
The problem with leprosy is the lack of a test to diagnose the disease. Unlike the various blood tests available to determine the presence of the disease or infection, leprosy is not diagnosed with a blood test. The only test available is that if someone suspects a skin lesion, a biopsy of the skin lesion can be done. In the event it is a case of a suspected leprosy patient, a ear lobe biopsy / smear can be done to determine the condition. This is mainly because these bacteria prefer to live in a cold environment and the ear lobe is deemed to be one of coolest area in the skin.
“Among the medical fraternity as well as laymen, there is a belief that leprosy is eradicated and is no more in Sri Lanka. We like to make it clear that leprosy is not eradicated and is still among us. Around 2,000 leprosy patients are reported in Sri Lanka every year. Hence, the Anti Leprosy Campaign’s slogan for this is year is ‘Leprosy is among with us’. Regardless of an age barrier, leprosy has affected lives of many including that of children. The problem is that children often meet with deformities as a result of leprosy. For an instance, if a child’s hand is affected with leprosy and presents with a nerve weakness, the child will not be able to use that hand for any effective function throughout life. Proper awareness needs to be raised among the public concerning this issue. People tend to neglect diagnosing leprosy since the general notion is that one has to make three to four visits to the doctor to make a diagnosis for leprosy, since many falsely tend to believe that the disease is actually a fungal infection. When the condition does not heal, finally the dermatologist will refer the person to do a skin biopsy where the diagnosis will be made” the doctor explained.
While treatment for leprosy is currently available in all Government hospitals free of charge, it should be noted that private hospitals do not provide their service for leprosy treatment. As Leprosy can be cured completely, patients with the condition should not be stigmatised. While patients with multibacillary type of leprosy should receive treatment for one year, paucibacillary type patients need to be treated for six months. When inquired if it is possible to have a recurrence of the disease once fully cured, he said that only a few such cases have been reported and such recurrences can be successfully avoided by following the treatment procedure properly without any negligence. “So far, we have not found any resistance to the treatment we administer to the patients in Sri Lanka. The multi drug treatment we provide has been very effective in treating patients” Dr. Piyasena said.
Take home message
When inquired about the take home message that could be given to the public, Dr. Piyasena reiterated that Leprosy prevails in Sri Lanka. Hence, it is important to seek immediate medical attention if one notices a skin rash or patch in one’s skin or if there is a tingling sensation in the fingers. In such event, the patient should go to a dermatology clinic to get himself/herself diagnosed and treated. “Leprosy is a condition that can be completely cured without causing any deformities and with less side effects,” concluded Dr. Piyasena .
19 Apr 2024 2 hours ago
19 Apr 2024 3 hours ago
19 Apr 2024 4 hours ago
19 Apr 2024 5 hours ago
19 Apr 2024 6 hours ago