Reply To:
Name - Reply Comment
Last Updated : 2024-04-25 18:55:00

 Arthritis is a general term used to describe inflammation of the joints.
Arthritis is a general term used to describe inflammation of the joints.
Osteoarthritis and Rheumatoid Arthritis (RA) are two disease types which are known to affect musculoskeletal system in several ways. Their prevalence in the modern society is quite high, but with timely interventions, the negative impact on the quality of life can be eliminated.
Since both these conditions own numerous similar signs and symptoms, they are often used interchangeably by people. So, from this article we are going to discuss what osteoarthritis and rheumatoid arthritis mean, their features, diagnosis and treatment, so that next time when a person you know is diagnosed with either of these diseases you will understand what it is exactly.
What is Osteoarthritis?
Also known as Arthrosis, osteoarthritis is a degenerative type of disorder which is known to be the commonest form of arthritis seen in the community.
It occurs as a result of wearing off of the protective cartilage at the end of joints over a period of time. This cartilage acts as a friction absorbing cushion and the absence of it can lead to a continuous friction generated on rubbing the bones with one another, ultimately ending up with a worn out joint.
Even though this condition can damage any joint in the body, the most commonly affected joints include hands, knees, hips and spine.
Advanced age, obesity, trauma to the joints, genetics, bone deformities (malformed/defective cartilage), long-term weight bearing and heavy weight lifters are more likely to get affected by osteoarthritis where females are at a higher risk than males in developing this condition. More often this affects people over 40 years of age, but it can also be seen in youngsters following accidents and trauma.
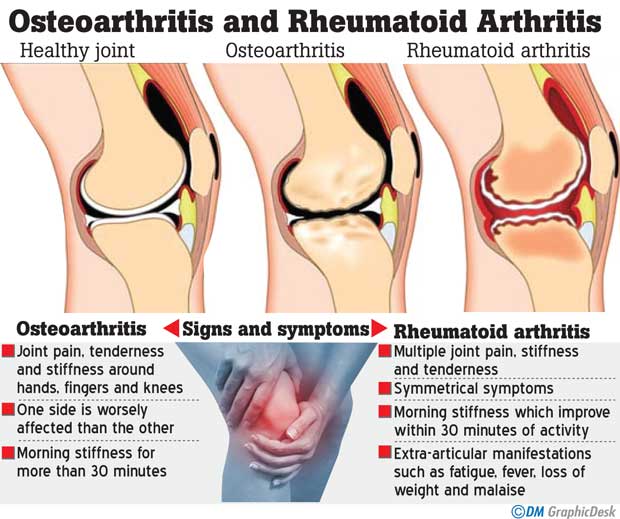
Patients with osteoarthritis usually present with Pain around the affected joints, difficulty in moving them due to stiffness and pain and stiffness which is aggravated more towards the morning just after waking up. This condition usually lasts for more than 30 minutes. In addition these people will also complain of loss of flexibility, limited range of movements, loss of muscle bulk, a grating sensation on moving joints and spurs which present as hard bony like structures over the skin around the affected joints.
Complications-Osteoarthritis should be diagnosed as early as possible failing which it can lead to a lifelong debilitating condition where the patients will no longer be able to work.
Your physician will ask for a complete history and do a thorough physical examination, looking for signs of inflammation such as pain, tenderness, swelling, redness and difficulty in moving before coming to a general diagnosis. However, this will further be confirmed by an X ray (worn off bones, absent cartilages and spurs could be seen) with or without an MRI. Furthermore, blood tests (ESR) and joint fluid analysis can also be important in order to exclude other mimicking conditions such as rheumatoid arthritis and gout respectively.
Even though, there is no complete cure for osteoarthritis, lifestyle modifications and pharmacological interventions are known to be able to address the condition in the aspect of symptoms.
1. Pain relief- Acetaminophen can be used for mild-moderate pain, but long term usage can lead to liver damage.
2. Non-steroidal anti-inflammatory drugs (NSAIDs) - Ibuprofen, Naproxen sodium
3. Anti-depressants such as Duloxetine- to treat chronic pain
1. Hyaluronic lubrication injections
2. Re-aligning bones
3. Joint replacement surgery or Arthroplasty- Removal of damaged joint surfaces and replacing them with metal or plastic parts.
What is Rheumatoid arthritis?
Rheumatoid arthritis is a chronic auto immune condition which is characterized by pain, tenderness, swelling and stiffness in the affected joints including hands, feet and wrists, in a symmetrical manner. This can also result in extra articular manifestations involving skin, eyes, lungs, blood and nerves.
Even though the exact etiology for rheumatoid arthritis is not clear, it is an autoimmune condition where the body produces antibodies against its own cells. Some scientists suggest that micro-organisms such as virus and bacteria play a major role in pathophysiology where smoking is thought to be another.
Accounting for a significant female predominance, Rheumatoid Arthritis usually affects young people around the age of 20.
The majority of the patients with Rheumatoid Arthritis present with an acute onset of joint pain, tenderness, swelling and limping in joints all over the body which will gradually progress as the weeks pass. Other extra articular symptoms can include fever, loss of appetite and weight, generalized body aches, red eyes, rheumatoid nodules over skin, anemia etc. Patients can also present with joint pains aggravated in the morning. This condition usually improve within 30 minutes in contrast to osteoarthritis pain.
Physicians are able to diagnose this condition by analyzing the signs and symptoms derived from a complete history along with information about the family background. This can be further confirmed using imaging studies such as X RAY and MRI along with blood tests such as Erythrocyte sedimentation rate (ESR), C-reactive protein (CRP) and cyclic citrulline antibody test (anti-CCP).
The treatment plan for Rheumatoid arthritis mainly includes lifestyle modifications and pharmacological interventions.
1. Anti-inflammatory agents
2. Pain relievers (Narcotics)
3. Corticosteroids
4. Disease-modifying anti-rheumatic drugs (DMARDs) – Hydroxychloroquine, Immuno-suppressants such as methotrexate
Even though there is no lifelong cure for Rheumatoid Arthritis, timely interventions can definitely prevent disability.
Where does the difference lie?
The major difference between these 2 conditions lies in the nature of the natural course. Even though both these conditions affect our musculoskeletal system, Osteoarthritis is a degenerative, wear and tear type disorder where RA is an autoimmune condition.
Both these conditions have a significant female predominance yet. Osteoarthritis usually affects people over 40 years of age where the incidence of RA is higher among young individuals around the age of 20.
Osteoarthritis is a result of long-term pressure on large joints such as hips, knee and elbow resulting in a wearing off where the exact etiology of RA is not very clear, suggesting the influence of a genetic predisposition and long term smoking.
Osteoarthritis usually affect one particular area or joint in the body where RA tends to affect multiple joints all over the body.
Summary Signs and symptoms Osteoarthritis
Rheumatoid arthritis
· Extra-articular manifestations such as fatigue, fever, loss of weight and malaise
Diagnosis
Treatment
References:
www.healthline.com
www.webMD.com

Add comment
Comments will be edited (grammar, spelling and slang) and authorized at the discretion of Daily Mirror online. The website also has the right not to publish selected comments.
Reply To:
Name - Reply Comment
US authorities are currently reviewing the manifest of every cargo aboard MV
On March 26, a couple arriving from Thailand was arrested with 88 live animal
According to villagers from Naula-Moragolla out of 105 families 80 can afford
Is the situation in Sri Lanka so grim that locals harbour hope that they coul